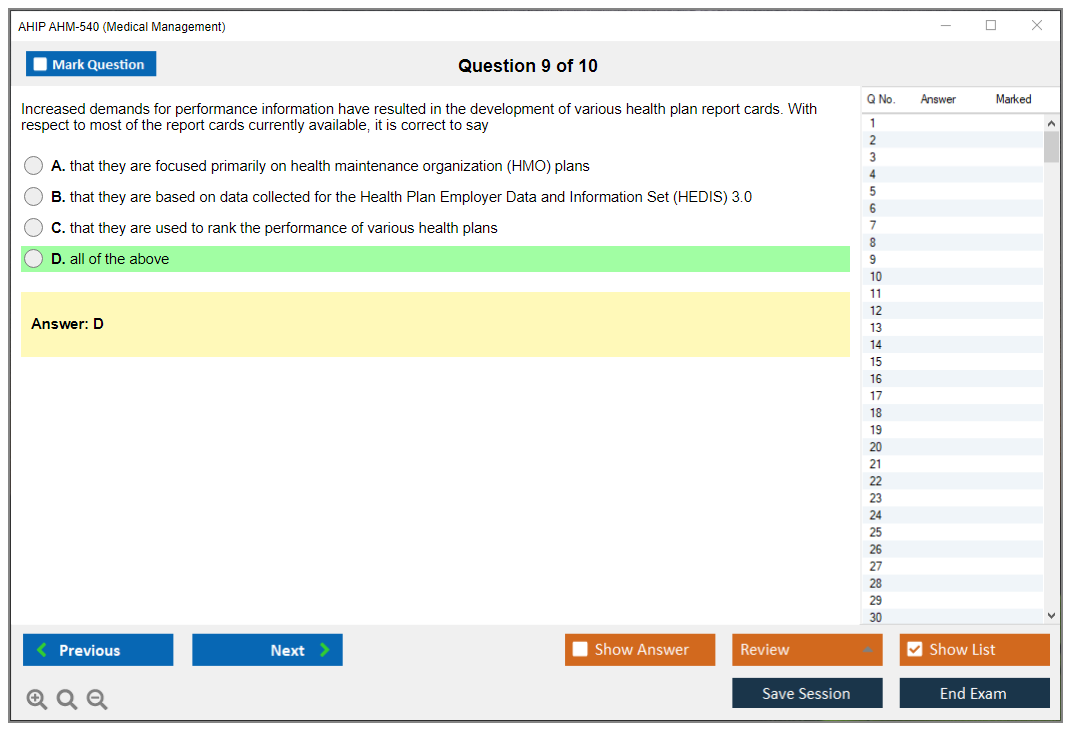
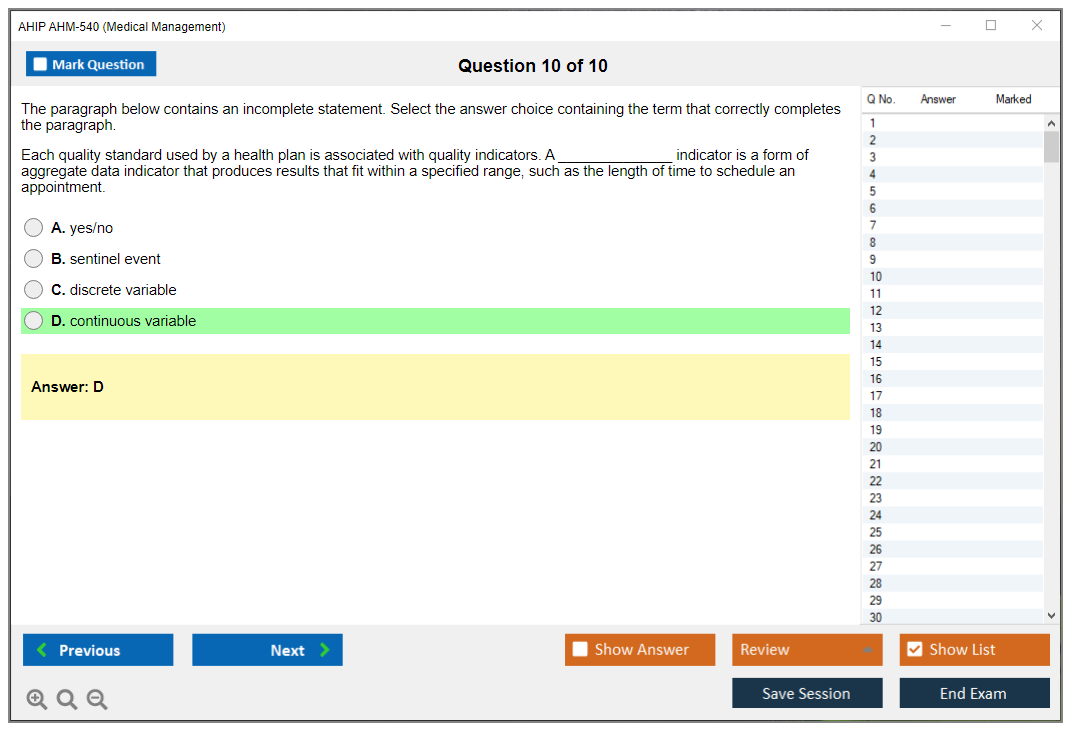
AHM-540 Practice Exam - Medical Management
Reliable Study Materials & Testing Engine for AHM-540 Exam Success!
Exam Code: AHM-540
Exam Name: Medical Management
Certification Provider: AHIP
Certification Exam Name: AHIP Certification

Free Updates PDF & Test Engine
Verified By IT Certified Experts
Guaranteed To Have Actual Exam Questions
Up-To-Date Exam Study Material
99.5% High Success Pass Rate
100% Accurate Answers
100% Money Back Guarantee
Instant Downloads
Free Fast Exam Updates
Exam Questions And Answers PDF
Best Value Available in Market
Try Demo Before You Buy
Secure Shopping Experience
AHM-540: Medical Management Study Material and Test Engine
Last Update Check: Mar 19, 2026
Latest 163 Questions & Answers
45-75% OFF
Hurry up! offer ends in 00 Days 00h 00m 00s
*Download the Test Player for FREE
Dumpsarena AHIP Medical Management (AHM-540) Free Practice Exam Simulator Test Engine Exam preparation with its cutting-edge combination of authentic test simulation, dynamic adaptability, and intuitive design. Recognized as the industry-leading practice platform, it empowers candidates to master their certification journey through these standout features.
What is in the Premium File?
Satisfaction Policy – Dumpsarena.co
At DumpsArena.co, your success is our top priority. Our dedicated technical team works tirelessly day and night to deliver high-quality, up-to-date Practice Exam and study resources. We carefully craft our content to ensure it’s accurate, relevant, and aligned with the latest exam guidelines. Your satisfaction matters to us, and we are always working to provide you with the best possible learning experience. If you’re ever unsatisfied with our material, don’t hesitate to reach out—we’re here to support you. With DumpsArena.co, you can study with confidence, backed by a team you can trust.
AHIP AHM-540 Exam FAQs
Introduction of AHIP AHM-540 Exam!
AHIP AHM-540 is an exam that tests a person's knowledge of health insurance and managed care. It is administered by the American Health Insurance Plans (AHIP) and is designed to assess a person's understanding of the principles and practices of managed care and health insurance. The exam covers topics such as managed care organization structure, health plan operations, health care delivery systems, and health care financing.
What is the Duration of AHIP AHM-540 Exam?
The AHIP AHM-540 exam is a two-hour exam.
What are the Number of Questions Asked in AHIP AHM-540 Exam?
There are a total of 60 questions on the AHIP AHM-540 exam.
What is the Passing Score for AHIP AHM-540 Exam?
The passing score required for the AHIP AHM-540 exam is 70%.
What is the Competency Level required for AHIP AHM-540 Exam?
The AHIP AHM-540 exam is a certification exam for health insurance professionals. It is designed to assess the knowledge and skills of individuals who work in the health insurance industry. The exam covers topics such as health insurance regulations, health care reform, health insurance products, and health care delivery systems. To pass the exam, individuals must demonstrate a comprehensive understanding of the health insurance industry and its related topics. The competency level required to pass the AHIP AHM-540 exam is intermediate.
What is the Question Format of AHIP AHM-540 Exam?
The AHIP AHM-540 exam has a single multiple-choice question format.
How Can You Take AHIP AHM-540 Exam?
The AHIP AHM-540 exam is available in both online and testing center formats. The online format requires candidates to create an account on the AHIP website, pay the exam fee, and then answer questions from a predetermined set of questions. The testing center format requires candidates to register for the exam at an approved Prometric Test Center, pay the exam fee, and then take the exam at the testing center.
What Language AHIP AHM-540 Exam is Offered?
The AHIP AHM-540 exam is offered in English.
What is the Cost of AHIP AHM-540 Exam?
The AHIP AHM-540 exam is offered for a fee of $199.
What is the Target Audience of AHIP AHM-540 Exam?
The Target Audience of the AHIP AHM-540 Exam is healthcare professionals such as case managers, physician advisors, utilization managers, and other health care professionals interested in gaining a better understanding of healthcare reimbursement.
What is the Average Salary of AHIP AHM-540 Certified in the Market?
The average salary for professionals with AHIP AHM-540 certification varies widely depending on their experience, industry, and geographical location. Generally, professionals with AHIP AHM-540 certification can expect to earn anywhere from $60,000 to $90,000 per year.
Who are the Testing Providers of AHIP AHM-540 Exam?
The American Health Insurance Plans (AHIP) does not provide testing for the AHIP AHM-540 exam. Candidates for the AHIP AHM-540 exam must self-study and register for the exam through the AHIP website.
What is the Recommended Experience for AHIP AHM-540 Exam?
The recommended experience for AHIP AHM-540 exam is at least three years of experience in the health insurance field. This experience should include knowledge of the Medicare Advantage and Part D programs and experience in areas such as marketing, operations, and compliance.
What are the Prerequisites of AHIP AHM-540 Exam?
The AHIP AHM-540 Exam has no prerequisites. However, AHIP recommends that candidates have at least a basic understanding of the healthcare industry and Medicare before attempting the exam.
What is the Expected Retirement Date of AHIP AHM-540 Exam?
The official website for AHIP AHM-540 exam is https://www.ahip.org/certification/. You can find the expected retirement date for the exam on this page.
What is the Difficulty Level of AHIP AHM-540 Exam?
The AHIP AHM-540 exam is considered to be of moderate difficulty. It requires a thorough understanding of the material and adequate preparation time to achieve a passing score.
What is the Roadmap / Track of AHIP AHM-540 Exam?
AHIP AHM-540 Exam is a certification track and roadmap for health insurance professionals. It is designed to help them understand the fundamentals of health insurance and how to apply them in their daily work. The exam covers topics such as health insurance terminology, health insurance plans, health insurance regulations, and health insurance claims processing. Passing the exam is a prerequisite to obtaining the AHIP AHM-540 certification.
What are the Topics AHIP AHM-540 Exam Covers?
The AHIP AHM-540 exam covers topics related to healthcare finance, reimbursement, and policy.
1. Healthcare Finance: This topic covers the fundamentals of healthcare finance, including the financial environment, financial accounting, and financial analysis.
2. Reimbursement: This topic covers the different types of reimbursement methods, including fee-for-service, managed care, and capitation.
3. Policy: This topic covers the different aspects of healthcare policy, including regulations, laws, and the impact of policy on healthcare organizations.
4. Risk Management: This topic covers the basics of risk management, including risk assessment, risk mitigation, and risk management strategies.
5. Quality Improvement: This topic covers the fundamentals of quality improvement, including quality assurance, quality improvement initiatives, and quality improvement tools.
6. Healthcare Information Technology: This topic covers the basics of healthcare information technology, including electronic health records, data analysis, and health information exchange
What are the Sample Questions of AHIP AHM-540 Exam?
1. What is the purpose of the Medicare Advantage Open Enrollment Period (MA OEP)?
2. What are the eligibility requirements for Medicare beneficiaries to enroll in a Medicare Advantage plan?
3. What are the differences between Medicare Parts A, B, and C?
4. How do Medicare Advantage plans differ from Original Medicare?
5. What are the requirements for Medicare Advantage plan renewals?
6. What are the benefits of enrolling in a Medicare Advantage plan?
7. How do Medicare Advantage plans coordinate with Medicare Part D prescription drug coverage?
8. What are the different types of Medicare Advantage plans?
9. What is the role of the Centers for Medicare & Medicaid Services (CMS) in regulating Medicare Advantage plans?
10. What measures must Medicare Advantage plans take to ensure quality of care for their members?
AHIP AHM-540 Medical Management Overview and Certification Value I've been working in healthcare IT for years now. The AHIP AHM-540 Medical Management certification keeps coming up in conversations with colleagues who've transitioned from purely technical roles into clinical operations or health plan management. It's one of those credentials that sits right at the intersection of clinical knowledge and business operations, which makes it pretty valuable if you're trying to move into medical management spaces. What this certification actually validates America's Health Insurance Plans administers the AHM-540. It focuses specifically on medical management principles within healthcare organizations. We're talking utilization management, case management, care coordination, quality improvement. Basically all the systematic approaches health plans use to make sure care's appropriate and cost-effective. It's recognized across health plans, managed care organizations, hospitals, and healthcare... Read More
AHIP AHM-540 Medical Management Overview and Certification Value
I've been working in healthcare IT for years now. The AHIP AHM-540 Medical Management certification keeps coming up in conversations with colleagues who've transitioned from purely technical roles into clinical operations or health plan management. It's one of those credentials that sits right at the intersection of clinical knowledge and business operations, which makes it pretty valuable if you're trying to move into medical management spaces.
What this certification actually validates
America's Health Insurance Plans administers the AHM-540. It focuses specifically on medical management principles within healthcare organizations. We're talking utilization management, case management, care coordination, quality improvement. Basically all the systematic approaches health plans use to make sure care's appropriate and cost-effective. It's recognized across health plans, managed care organizations, hospitals, and healthcare consulting firms.
What makes this different from generic healthcare certifications is the specificity. You're not learning broad healthcare concepts. You're diving into how health plans actually operate their medical management programs, how they evaluate medical necessity, how they coordinate care for high-risk populations. It's part of AHIP's broader certification ecosystem, sitting alongside credentials like AHM-520 for health plan finance and AHM-530 for network management.
The credential fits with current healthcare trends. Value-based care. Accountable care organizations. All that transformation stuff happening in the industry. Which means it's not teaching you outdated fee-for-service approaches. Actually relevant to how healthcare's moving.
I remember sitting in a meeting last year where a consultant kept throwing around "care continuum" without understanding how utilization review actually functions at each point. Guy had an MBA but couldn't explain why concurrent review matters differently than retrospective. That's the gap this certification tries to fill.
Who actually benefits from pursuing this
Utilization management nurses? They're the obvious candidates. If you're doing pre-authorization or concurrent review work, this formalizes what you're already doing and gives you the theoretical framework behind it. Case managers go after this too, especially those coordinating care for complex patient populations where you need to understand the broader medical management context.
Medical directors overseeing clinical programs find value here. Quality improvement specialists focused on HEDIS measures and NCQA standards. Population health managers developing chronic disease programs. Healthcare administrators trying to transition into medical management leadership.
Mid-career professionals looking to formalize their expertise with recognized credentials make up a big chunk of test-takers. You might have five years of experience in utilization review, but without a credential, you're competing against people who have both experience AND certification. Clinical consultants advising health plans also pursue this to demonstrate they actually understand medical management program design.
Career impact and professional value
Here's the thing about credentials in healthcare. They don't guarantee you a job, but they absolutely boost credibility when you're applying for medical management and utilization review positions. Look at job postings for medical management roles. Many list AHIP certifications as preferred qualifications, and some even require them for senior positions, which honestly makes sense when you think about the complexity involved.
The systematic framework you gain? Probably more valuable than the credential itself. You learn how medical management works across the care continuum, not just in your specific silo. You understand regulatory requirements including URAC and NCQA accreditation standards, which matters when your organization's going through accreditation or trying to improve quality scores.
Salary ranges? Credentials can qualify you for higher brackets. But the bigger value's in your ability to communicate with clinical teams, payers, and healthcare executives using a common language and framework. You're not just saying "we need better utilization management." You're explaining specific methodologies and approaches that're industry-recognized.
For professionals in Medicare Advantage, Medicaid managed care, commercial health plans, this keeps you current on evolving methodologies. Healthcare changes fast. What worked three years ago doesn't necessarily work now.
How AHM-540 fits with other certifications
The AHM-540 complements other AHIP credentials pretty well. If you've already done AHM-250 as an introduction to healthcare management, the 540 goes deeper into the medical management piece specifically. It pairs nicely with AHM-510 for governance and regulation if you're trying to understand the compliance side.
You can pursue it standalone or as part of a broader development pathway. A lot of people combine it with case management certifications like CCM or utilization review credentials for maximum impact. I've seen nurses with clinical backgrounds use this to gain business and operational knowledge, while business-side folks use it to build clinical management competencies.
The integration's what matters. Medical management drives both financial and quality outcomes in health plans, so understanding how those pieces connect makes you way more effective in your role.
Medical management in the health plan context
Medical management isn't just about saying no to services. It's systematic approaches to ensuring appropriate, cost-effective care delivery.
Utilization management processes evaluate medical necessity before, during, and after care. Pre-authorization. Concurrent review. Retrospective review.
Case management targets high-cost, complex patients who need intensive care coordination because they're juggling multiple conditions, multiple providers, social barriers to care.
Population health management strategies target specific conditions and risk cohorts. You're not managing individual cases. You're managing populations of diabetics or people with congestive heart failure.
Care coordination across settings reduces fragmentation and improves transitions. Hospital to home. Specialist to primary care. All those handoffs where things typically fall apart.
Quality improvement methods boost outcomes and patient experience while addressing regulatory compliance with state and federal requirements. The balancing act between clinical appropriateness and cost containment in a value-based care environment is where the real skill comes in. You can't just cut costs. You need to maintain or improve quality while managing utilization.
Why this matters right now
Rising healthcare costs're driving increased focus on medical management effectiveness. Health plans that do this poorly lose money and have bad quality scores. Plans that do it well succeed financially and clinically.
The shift toward value-based payment models? Requires sophisticated utilization and quality management. You can't wing it anymore. Growing Medicare Advantage enrollment's creating massive demand for skilled medical management professionals who understand that population. Medicaid expansion and managed Medicaid programs need specialized population health expertise because you're dealing with complex social determinants of health.
Regulatory scrutiny of prior authorization processes means you need compliant, evidence-based approaches. You can't just deny stuff arbitrarily. Social determinants of health integration's expanding the scope of medical management programs. Now you're addressing housing, food insecurity, transportation barriers. Technology advances including predictive analytics and AI're boosting capabilities, but you need to understand the fundamentals to use those tools effectively.
What you actually learn
After earning the AHM-540, you should have solid understanding of medical management program design and implementation. You can develop and evaluate utilization management criteria and processes. You understand different case management models and when to apply them.
Quality measurement, reporting, and improvement methods make sense. Population health approaches for chronic condition management become part of your toolkit. You're aware of regulatory, ethical, and compliance considerations that govern what you can and can't do.
The analytical skills for evaluating program effectiveness matter too. Can you look at data and determine if your utilization management program's actually working? Can you identify where care coordination's breaking down? Can you lead cross-functional teams that include clinicians, IT staff, operations people, and executives?
That's what the certification's supposed to prepare you for. Whether it actually does depends on how much effort you put into studying and applying the concepts, not just memorizing answers for the exam.
AHM-540 Exam Objectives and Content Domains
Quick orientation on what this exam is about
AHIP AHM-540 Medical Management is basically the "how health plans run clinical operations" exam. Not theory-only. It expects you to understand how medical management concepts in health plans turn into day-to-day decisions like prior auth workflows, inpatient concurrent review, case management outreach, and quality reporting that can survive an audit.
This is the test for people who sit between clinical care and plan economics. Nurses in UM/CM. Analysts supporting population health. Provider relations folks who keep hearing "why'd you deny this?" and want a real answer.
What the content domains actually cover
You get hit with five big buckets plus compliance. The tricky part is how connected they are. You can memorize definitions, but the exam keeps nudging you toward "what happens next" in a process, who owns which decision, and what documentation proves you did it correctly.
Medical management foundations and core concepts
Medical management starts as managed care's way to control inappropriate utilization, then evolves into something closer to clinical operations for value-based care. Same bones, different posture. The exam likes that evolution story. It also likes frameworks like the Triple Aim (population health, patient experience, cost) and the Quadruple Aim, where provider and staff experience gets added because burnout wrecks quality and access faster than any policy memo fixes it.
Definitions matter. Short ones. Medical necessity matters. Documentation matters.
You should know how medical management supports ACOs and value-based contracts, where the plan tries to align clinical quality, cost management, and patient satisfaction objectives without creating chaos for providers. Evidence-based medicine shows up here too, mostly through clinical practice guidelines and how they feed criteria and care pathways. Expect questions about how criteria get built, updated, and applied, and why you cannot just "go with gut" when members appeal.
Network management and contracting shows up more than people expect. If your network contract has prior auth rules, referral requirements, or site-of-care steerage, medical management ends up enforcing it, and that relationship can get tense when providers think UM is "just denial." Data analytics also lives in this domain: predictive modeling for high-risk populations, care gap identification, and the tech stack behind it like authorization platforms and case management software.
Program evaluation is part of foundations too. Not a spreadsheet-only thing. Think performance monitoring, stakeholder engagement (providers, members, regulators), and metrics that prove a program improved outcomes rather than just moved cost around. I spent six months in quality improvement once where we celebrated a "cost-neutral" intervention, and management looked at us like we'd insulted their mothers. Turns out improved outcomes without increased cost is actually a win when you're dealing with complex chronic conditions, but try explaining that in a budget meeting.
Utilization management principles and processes
UM is the most testable process domain because it is structured and regulated. Prospective review is your prior authorization and pre-cert workflow, where the plan evaluates medical necessity before services happen. You need to be clear on who initiates it, what information is required, and what happens when it is incomplete.
Concurrent review is about inpatient stays and ongoing treatment episodes. Daily or periodic touchpoints. Level of care. Length of stay. Discharge planning. Transition management is not "someone else's problem." UM and discharge planning are tied together because a bad discharge plan creates readmissions and ED bounce-backs, and then your utilization metrics look awful.
Retrospective review shows up for claims payment, quality assurance, and sometimes fraud, waste, and abuse signals. Different intent. Different timing. Same need for defensible criteria.
Criteria sources matter, and the exam calls them out: MCG, InterQual, and proprietary guidelines. You do not need vendor trivia, but you do need to know why standardized criteria helps with consistency and appeal defensibility, and where a physician advisor gets pulled in for complex determinations, especially when the clinical story does not fit neatly into a criteria box.
Appeals and grievances. Timelines. Notices. External review. This is where state insurance rules and CMS requirements bite. URAC accreditation standards also show up, mostly around program structure, decision timeframes, and member communication requirements.
A few operational concepts tend to pop on AHM-540 exam objectives: peer-to-peer reviews, gold carding for high-performing providers, and prior authorization automation. Automation is not magic. It is rules engines, clean data, and exception handling, and if any of those are messy, nurses and physician advisors end up cleaning it up at 4:45 pm on a Friday.
Case management and care coordination strategies
Case management is where "utilization management vs case management" finally clicks. UM is episode and service focused. CM is person focused over time. Different lens. Different success measures. Telephonic case management, field-based, embedded in clinics, and transitions-of-care models all show up, and you should know what each is good for and what it costs to run.
Identification and stratification is a major theme: predictive analytics, claims triggers, pharmacy signals, frequent ED use, rising-risk cohorts. Then assessment: clinical, functional, psychosocial, and environmental factors. Not a checkbox exercise. Fragments matter here. Housing. Food. Transportation. Caregiver support.
Care planning follows, with member-centered goals, interventions, and measurable follow-up. Complex case management includes catastrophic illness, multi-morbidity, and high-cost conditions, while disease management is more standardized for conditions like diabetes, heart failure, COPD, and asthma.
Motivational interviewing and health coaching show up because plans cannot "order" behavior change. They can only influence it. Documentation and privacy considerations matter here too because case notes are discoverable, regulated, and often shared across teams with minimum necessary rules under HIPAA.
Competencies matter. CCM and ACM are common. Continuing education is not fluff, especially when guidelines and drug therapy change faster than internal policy manuals.
Outcomes measurement includes cost savings, quality improvements, and member satisfaction, but also continuity and reduced readmissions when transitions-of-care is done right. Behavioral health integration is part of whole-person care, and the exam expects you to understand why separating medical and behavioral workflows can create blind spots, medication issues, and duplicated outreach that members hate.
Quality improvement and outcomes measurement
Quality is where the plan proves it is paying claims. HEDIS measures, CAHPS patient experience, and Medicare Advantage Star Ratings come up repeatedly. NCQA accreditation standards too, and you should be able to connect the dots between "we run this program" and "we can report it cleanly and validate it."
Methodologies like PDSA cycles are fair game. Six Sigma and Lean principles show up more as concepts than math. Performance improvement projects (PIPs) are big in Medicaid managed care, and root cause analysis shows up for adverse events and quality gaps.
Provider profiling and feedback. Touchy topic. Necessary topic. Pay-for-performance programs tie quality metrics to reimbursement, which loops you right back to contracting and network management from the foundations domain. Health equity and disparities reduction is increasingly baked into QI, so expect questions that connect stratified reporting, culturally appropriate outreach, and closing gaps for specific populations rather than "average improvements."
Data validation and audits matter because bad data equals bad reporting, and bad reporting equals sanctions, corrective action plans, and leadership panic.
Population health management approaches
Population health is the "zoomed out" layer. Segmentation and risk stratification. Preventive care. Chronic disease programs. Maternity and neonatal management. Pediatric considerations including EPSDT. The exam usually tests the logic of it: find risk, identify care gaps, engage members and providers, measure results.
High-risk population identification uses predictive modeling and claims analytics, but also human referral pathways from providers and care managers. SDOH integration is not optional anymore. Health risk assessments and biometric screening can feed outreach programs, and pharmacy management integration matters because adherence is one of the easiest ways to lose control of outcomes and cost.
Technology platforms show up again: population health tools, registries, member portals, outreach systems. The point is coordination at scale, without spamming members or confusing providers.
Regulatory, ethical, and compliance considerations
This domain is where people lose points because they "kind of know it." HIPAA privacy and security requirements, state insurance regulations for UR and appeals, CMS rules for Medicare Advantage and Medicaid MCOs, and ACA provisions like preventive services and essential health benefits are all in scope.
Mental Health Parity and Addiction Equity Act compliance matters for behavioral health management. Network adequacy standards matter for access. External review processes matter for denied services and experimental or investigational determinations. Fraud, waste, and abuse shows up as detection and prevention, and ethical considerations show up around medical necessity decisions, resource allocation, and conflicts of interest in incentive structures.
Cultural competency and health literacy matter in member communication. So do documentation and record retention requirements. Boring. Tested.
The practical exam questions people keep asking
How much does the AHM-540 exam cost? It depends on AHIP's current pricing and whether your employer buys a bundle, so check the official AHIP Academy page for the latest AHM-540 exam cost.
What is the AHM-540 passing score? AHIP does not always present scoring the way people expect, so confirm the current AHM-540 passing score policy in your candidate handbook or course portal.
How hard is the AHM-540 Medical Management exam? AHM-540 exam difficulty is moderate if you have worked UM/CM/QI, and annoying if you have not, because the questions assume you understand workflows, compliance rules, and why a plan would choose one intervention over another.
What are the best AHM-540 study materials and practice tests for AHM-540? Start with official AHM-540 study materials from AHIP, then add an AHM-540 practice test only if it matches current objectives and forces you to review rationales, not just memorize answers.
Are there AHM-540 prerequisites or renewal requirements? Formal AHM-540 prerequisites can be light, but the recommended background is real-world exposure to managed care operations, and AHM-540 renewal requirements, if applicable to your credential path, should be verified on AHIP's current recert rules since they change more often than people think. Nobody reads those updates until their credential lapses and then it is a scramble.
AHM-540 Prerequisites and Eligibility Requirements
No formal barriers but practical reality matters
AHIP doesn't gatekeep. There's no requirement you've passed AHM-250 or any other exam first. No medical degree needed. You don't even need a bachelor's degree, though, okay, hold that thought. We'll circle back to why that actually matters in a minute.
Registration? Dead simple. You create an account on the AHIP or AHIP Academy platform, pay your fee, done. Some folks snag discounted access through their employer's group purchase or through professional memberships in healthcare organizations, which honestly seems like the smarter play if you can swing it. I've seen companies buy entire educational packages that include AHM-540 along with other certifications like AHM-520 (Health Plan Finance and Risk Management) or AHM-530 (Network Management).
You'll need to verify your identity during registration and exam proctoring. That's non-negotiable, and yeah, they're serious about it. International candidates can absolutely take the exam, but the thing is, the content is heavily U.S.-focused. Medicare regulations, Medicaid standards, American healthcare delivery models that just don't exist elsewhere. If you're managing care in Toronto or London, you'll still learn valuable concepts, sure, but the regulatory specifics won't transfer directly and that might frustrate you.
What actually helps you succeed
Here's where it gets real.
No prerequisites? Sure. But should you just jump in cold? Not gonna lie, that's a rough path and I wouldn't recommend it.
One to three years working in healthcare operations makes a massive difference in ways that're hard to quantify but impossible to ignore. If you've been in managed care, utilization review, case management, or even clinical settings with exposure to authorization processes, you're already miles ahead of someone coming in fresh. You know what a prior auth is without Googling it. You've seen denial letters and the headaches they cause. You understand why a health plan might question a three-day inpatient stay for something that could realistically be outpatient, and you get the financial and clinical reasoning behind that pushback.
Familiarity with health insurance terminology helps enormously. Premiums, deductibles, copayments, coinsurance, out-of-pocket maximums. If those terms make you pause even for a second, you'll burn study time on basics instead of the medical management concepts that actually get tested. Same with provider networks, claims processing, and how utilization management fits into the bigger operational picture.
Clinical professionals like RNs, MDs, PAs, or therapists? Huge advantage with the medical content, honestly. They already know disease states, treatment protocols, medication classes inside and out. A nurse who's done bedside care for five years doesn't need to memorize what CHF stands for or why someone with poorly controlled diabetes might need case management. It's second nature. Non-clinical folks need to supplement heavily with healthcare terminology and clinical basics before even cracking the study guide. That's just reality, no way around it.
Knowledge gaps you should address before studying
The exam assumes you understand healthcare delivery systems without explaining them. Inpatient versus outpatient settings. Post-acute care settings like SNFs and home health agencies. If you've never worked in healthcare, these distinctions aren't intuitive and they're not always logical.
You should know basic health insurance concepts beyond just memorizing the terms. How do payment models work in practice? What's capitation versus fee-for-service? Why does a health plan care about readmission rates beyond just quality scores? The AHM-540 Practice Exam Questions Pack for $36.99 can expose these gaps pretty quickly, but honestly you're better off addressing them before you start formal study or you'll waste time.
Medical terminology matters more than people think it should. The exam won't define every clinical term. They assume baseline knowledge. You'll see questions about appropriateness of care for specific conditions, and if you don't know what an MI is, or why someone post-CVA might need intensive case management, you're essentially guessing. Common disease states, standard treatments, typical procedures. These should be at least somewhat familiar territory.
Quality measurement comes up repeatedly, maybe more than you'd expect. Performance metrics and what they actually measure. HEDIS measures and why they matter. Clinical outcomes versus process measures and the philosophical difference between them. You don't need to memorize every HEDIS spec, but you should understand why health plans measure things like diabetic eye exams or beta-blocker use post-MI.
The regulatory environment? Unavoidable.
Medicare and Medicaid operate under completely different rules and funding structures. Commercial insurance has different requirements altogether. The exam tests whether you understand how regulations shape medical management decisions in real-world scenarios, not just theory. Evidence-based medicine and clinical guidelines underpin the entire field. If you're not comfortable with how clinical practice guidelines get developed and applied in actual care settings, that's a study priority you can't skip.
Funny thing is, I once talked to someone who thought "evidence-based" just meant "whatever the doctor decides." That's..not quite it. The whole point is using research and data to drive decisions, not gut feelings or tradition. Anyway.
Educational background helps but isn't everything
A bachelor's degree in healthcare administration, nursing, public health, or related fields definitely helps smooth the path. You've already been exposed to healthcare systems thinking and the frameworks that drive decision-making. Clinical degrees provide that strong medical foundation I mentioned earlier, which saves you tons of study time. An RN studying for AHM-540 can focus almost exclusively on the management and regulatory aspects because the clinical content is familiar territory they've lived.
Business degrees like an MBA or MHA give you the operations and strategic perspective that's harder to pick up on the job. You understand organizational dynamics, financial drivers, performance management frameworks. That's valuable when the exam asks about implementing a new utilization management program or measuring ROI on case management interventions. You already think that way.
But I've seen non-degreed professionals with ten years in healthcare absolutely crush this exam and outscore people with advanced degrees. Experience counts, sometimes more than formal education. If you've been a case manager without formal credentials, or worked in UM for years, you have practical knowledge that textbooks can't teach and that shows up in scenario-based questions.
Complementary certifications help too, and they're worth pursuing if you're career-focused in this space. CCM (Certified Case Manager), ACM-RN, CPHQ. These provide overlapping knowledge that reinforces what you're studying. If you're studying for AHM-540 and you already have CCM, you'll recognize care coordination concepts immediately and that familiarity builds confidence.
Skills that matter beyond healthcare knowledge
Analytical thinking is huge for this exam. The exam presents complex scenarios. A patient with multiple comorbidities, conflicting treatment recommendations from different specialists, cost considerations that can't be ignored, quality metrics that must be met. You need to evaluate all the factors at once and identify the most appropriate medical management approach without getting paralyzed by the complexity.
Attention to detail? That separates passing from failing more often than knowledge gaps do. Regulatory requirements have specific language that matters legally. Processes have defined steps that can't be skipped. Miss a key word in a question stem and you'll pick the wrong answer even if you know the content cold. I've seen it happen repeatedly.
Critical thinking means applying concepts to new situations you haven't specifically studied. The exam won't just ask you to regurgitate definitions from the textbook. You'll get case studies that feel pulled from real medical management departments. Real-world scenarios with messy details. "What should the case manager do next?" requires understanding principles well enough to apply them flexibly, not just memorize protocols.
Reading comprehension matters more than people expect going in. Dense regulatory text that requires careful parsing. Clinical documentation with relevant details buried in paragraphs. Multi-paragraph scenarios where the question stem itself is three sentences long. If you struggle with sustained focus while reading technical material, practice that separately before exam day.
Time management applies both to studying and test-taking, and both require discipline. Can you carve out consistent study time over weeks or months? During the exam itself, can you pace yourself to answer all questions without rushing the last third or getting stuck on difficult items?
Timing this certification in your career path
Early-career professionals use AHM-540 to build foundation knowledge when they're still figuring out their specialty. You're establishing yourself in medical management, and the credential signals you've invested in formal education beyond on-the-job learning, which matters to hiring managers.
Mid-career transitions are common, maybe the most common reason people pursue this. A bedside nurse moving into utilization review who needs credibility in the new role. A social worker shifting to case management and wanting structured learning. A claims analyst moving to clinical operations and filling knowledge gaps. The certification provides structure for learning the new domain and looks great on a resume during transition periods.
I mean, if you've been doing medical management for fifteen years without formal credentials, AHM-540 validates what you already know, and that matters even if it feels redundant. Some organizations require or prefer certified staff for certain positions or pay grades. Getting the credential removes that barrier to advancement or lateral moves.
Before applying for medical management jobs, the certification strengthens your candidacy in ways that're hard to measure but obvious in interviews. Employers see you've proactively learned the field rather than expecting to be trained from scratch, and that initiative stands out when they're comparing candidates.
If your employer offers tuition reimbursement or professional development budgets, that's your signal. Use it now. The AHM-540 Practice Exam Questions Pack at $36.99 is a minimal investment compared to the exam fee and course materials, and it's a smart diagnostic tool.
Six months to a year in a medical management role provides practical context that makes studying more effective and less frustrating. You've seen the concepts in action on real cases. Questions make sense because you've lived the scenarios, not just read about them. Starting AHM-250 (Healthcare Management: An Introduction) might make sense if you're completely new to healthcare, like zero exposure, then progressing to AHM-540 once you have some foundation and context.
Some people pursue multiple AHIP certifications as part of a broader credential plan that spans years. AHM-540 pairs well with AHM-510 (Governance and Regulation) if you're moving into compliance or leadership roles where regulatory knowledge is necessary. The knowledge builds on itself across the certification series, creating compound returns on your study investment.
AHM-540 Exam Cost and Fee Structure
Quick overview of AHIP AHM-540 (Medical Management)
Look, AHIP AHM-540 Medical Management sounds cushy at first, until you're neck-deep in the actual language health plans use to run care programs, approve services, and defend decisions when auditors come knocking. It's medical management concepts in health plans, but there's enough policy, process, and measurement talk that you can't just coast through on clinical instincts alone.
Some content? Straightforward. Other parts are annoyingly specific, honestly.
What the course actually covers
Medical management's the big umbrella here, and AHM-540 drills into how plans think about the entire flow from request to decision to outcome. You'll see utilization management versus case management come up constantly, plus all the stuff that glues it together like care coordination and quality improvement initiatives.
Here's what you're studying:
- utilization management basics, prior auth logic, and where UM fits in a plan's operations (this part matters because the exam likes process steps and definitions, not just "UM reduces cost")
- case management workflows and care coordination, risk stratification ideas, and how nurse-led programs get evaluated over time
- quality improvement and outcomes measurement, including why plans obsess over metrics, documentation, and audit trails
- population health management strategies, chronic condition programs, how interventions get targeted
- compliance and ethics, because honestly AHIP exams always want you thinking about regs and member protections
Not everything needs deep memorization. Definitions though? Yeah, those do.
Who should take it
If you're in UM, CM, appeals or grievances, quality, population health, provider relations, or even analytics supporting those teams, AHM-540 lines up well. Trying to move from clinic life into payer work? This credential can help you talk like the hiring manager, which matters more than people admit.
Also. Employer already likes AHIP? That changes everything, honestly.
Why people earn the credential
Resume signal. That's one reason.
It's also internal credibility when you're sitting in a meeting arguing about medical necessity language, escalation paths, or why a care coordination program didn't move readmission rates the way everyone expected it to.
And yeah, sometimes it's just required for the job ladder. Not glamorous, but real.
I once sat through a VP-level budget meeting where someone without medical management credentials kept getting cut off mid-sentence whenever utilization targets came up. Not fair maybe, but the person with AHIP designations on their email signature got listened to every single time. Credentials create breathing room in conversations like that.
What you'll be tested on (AHM-540 exam objectives)
AHM-540 exam objectives usually read like a table of contents for a health plan's medical management department. The exam tends to reward people who can separate concepts cleanly: UM versus CM, administrative denials versus clinical denials, quality measurement versus program operations, population health versus individual care planning.
A few areas that show up as gotchas:
- the boundaries between departments, who does what, and when something gets escalated
- program evaluation language, because outcomes measurement isn't the same as activity tracking
- compliance framing like member rights, documentation, and consistent application of criteria
The thing is, none of this is impossible. But it's easy to overstudy the wrong thing if you don't map your notes to the objectives early.
Prerequisites and eligibility (what's real vs what's implied)
AHM-540 prerequisites are usually more "recommended" than "you must have X degree." AHIP generally expects you to be comfortable with health insurance basics, medical management workflows, and healthcare terminology. Not rocket science, but not ignorable either.
Recommended background
If you've worked with authorizations, concurrent review, discharge planning, case management, appeals, HEDIS-adjacent metrics, or population programs, you'll feel at home. Haven't worked in those areas? You can still pass, but you'll spend more time building context from scratch.
Account or enrollment requirements
You'll typically need an AHIP or AHIP Academy account, and some people get access through an employer portal. That's where membership status or organizational affiliations can change pricing and access.
Suggested prior knowledge areas
Know the difference between utilization review tasks and case management tasks. Know how quality improvement gets measured. Know the basics of care models and chronic condition management.
Foundation stuff, really.
Exam registration cost (what to expect)
AHM-540 exam cost is usually the first thing people ask, honestly, it's because budgets are tight and employers love reimbursement rules with seventeen conditions attached.
Standard exam registration fees commonly fall in the $200 to $400 range for individual registration, but you should verify current pricing on the AHIP website because "pricing subject to change" isn't a cute disclaimer, it's real life with these programs. Pricing may shift based on AHIP membership status or organizational affiliations, and that's especially true if your employer has an agreement that routes you through a different catalog or bundle altogether.
Exam fee generally covers one attempt. Course materials may be bundled with exam fee or purchased separately, which is where people accidentally overspend. They assume the training and the test are automatically packaged, then get surprised at checkout.
Payment typically required at time of registration via credit card or organizational purchase order. After successful payment processing, you'll usually get a confirmation email with exam access details, and that email is basically your receipt and your "don't panic, you're enrolled" proof all in one.
Retake fees and policies (aka the part nobody wants)
Failed exam attempts require purchasing retake at additional cost. Retake fees typically similar to original exam registration cost. Not always identical, but close enough that you should budget like you might pay twice if you're going in cold or distracted.
Waiting period? Often required between exam attempts, often 14 to 30 days. Unlimited retakes available in many cases, but each requires separate fee payment, so "unlimited" isn't comforting, it's just expensive if you keep failing.
Some packages include one free retake or a discounted retake option, and if you see that offered, it can be worth it if you're unsure about AHM-540 exam difficulty or you're rushing prep because life got crazy. Previous exam results and score reports are usually accessible. You should actually use them, I mean strategic retake preparation using score reports to target weak areas is the only sane way to approach round two.
If your study materials were bundled, they often remain accessible between attempts. Bought them separately? Double-check access windows so you don't get locked out right when you're trying to retake.
Discounts, bundles, and cost-saving options
There are a bunch of ways people pay less, but not all of them apply to everyone, which is frustrating when you're hunting for savings.
Common options you might run into:
- AHIP organizational memberships that provide discounted exam access for employees (this is the big one, ask your training department)
- multi-exam bundles that reduce the per-exam price if you're stacking certifications
- AHIP Academy annual subscriptions that may include access to AHM-540 and other courses and exams (worth it if you're doing more than one)
- group purchasing discounts for employers registering multiple employees
- professional association member discounts through partnerships with AHIP
- student discounts for healthcare administration programs
- early registration discounts for certain windows
- promo periods around conferences
If I had to pick two to actually investigate first: employer access and Academy subscription. Those are the ones that move the needle, and the rest are more "nice if you qualify" situations.
Employer reimbursement and sponsorship (how to not pay out of pocket)
Many healthcare organizations reimburse professional development and certification costs, but they can be picky about timing and conditions. Request pre-approval from your manager or HR before registering, because a lot of policies won't reimburse if you paid first and asked later. Yeah, it's backwards, but that's corporate policy for you.
Document the business case in plain language: how AHIP AHM-540 Medical Management maps to your current role, how it supports organizational objectives like improved throughput, better care coordination and quality improvement, fewer avoidable admissions, cleaner audit performance, that kind of thing. Some employers require a passing score for reimbursement, so understand policy before registering, and don't assume you'll get paid back if you fail on the first try.
Professional development funds might be annual budgets or education allowances. Tuition assistance programs at larger health plans often cover AHIP certifications specifically. Also, negotiate certification support during a job offer or performance review, because honestly that's when budgets magically appear from nowhere.
Track all expenses. Exam fee, study materials, practice tests. Every receipt matters.
Extra costs beyond the exam fee (budget like an adult)
The exam fee isn't always the full bill, which catches people off guard. Official AHIP study materials and textbooks might cost extra if not included in your bundle. Supplemental study guides, reference books, or online courses add up fast, especially if you panic-buy stuff the week before your exam date.
Practice exams and question banks from third-party providers can help, but choose carefully based on reviews. If you want something targeted, I've seen people use the AHM-540 Practice Exam Questions Pack as a lightweight way to pressure-test weak areas without committing to another full course that you'll never finish anyway. If you do buy extra prep, be intentional, and don't stack five resources you'll never actually open.
There's also the time cost, which people forget. If you're taking unpaid study leave or you're reducing billable hours to prep, that's real money walking out the door. Testing center fees might apply if in-person proctoring is required, though most AHIP exams are online now, and you'll need technology requirements like a reliable computer, webcam, and stable internet for online proctored exam sessions.
Future you also pays. AHM-540 renewal requirements or recertification fees can pop up later depending on AHIP policy and credential maintenance rules at the time, so factor that into the long-term math.
Passing score, difficulty, and study approach (what people actually ask)
AHM-540 passing score rules can vary by exam version and policy, so confirm in your candidate handbook or AHIP portal. Score reports and result timing also vary, but you typically get enough feedback to identify weak domains, which matters if you're retaking.
How hard is it? AHM-540 exam difficulty is moderate if you've worked in a plan, and harder if you're coming from purely clinical settings because the exam wants "plan logic," not bedside logic, and it expects you to respect process and documentation even when you personally disagree with it, which can feel, I mean, it can feel unnatural at first.
For AHM-540 study materials, start with official course content if you have it, then add a practice layer on top. AHM-540 practice test work is where you find out if you actually understand the definitions and scenarios versus just recognizing terms, and that's why a focused resource like the AHM-540 Practice Exam Questions Pack can be useful near the end, especially if you're trying to study around a full-time job and family obligations.
FAQ style answers people search for
How much does the AHM-540 exam cost? Usually $200 to $400 for individual registration, but verify current pricing on the AHIP website before you commit.
What is the passing score for AHM-540? It depends on AHIP's current scoring policy for that exam form, so check the official details in your portal or candidate handbook.
What are the best study materials and practice tests for AHM-540? Start with AHIP materials as your foundation, then add targeted practice like the AHM-540 Practice Exam Questions Pack if you want extra question reps to build confidence.
Are there prerequisites or renewal requirements? AHM-540 prerequisites are mostly recommended background, and renewal requirements can change over time, so confirm the current rules before you commit to the certification path.
AHM-540 Passing Score and Scoring Methodology
What you actually need to score
Look, AHIP doesn't publish an exact AHM-540 passing score publicly, which honestly drives people nuts. Most candidates report needing somewhere between 70-75% to pass, but the thing is, that's not carved in stone. The scoring methodology uses scaled scoring, meaning your raw score (how many questions you got right) gets converted to a scaled score that accounts for question difficulty and exam version variations.
What this means in practice: you can't just count questions and know whether you passed. Two people might answer different questions correctly but get the same scaled score because AHIP weights questions differently. Frustrating when you're sitting there trying to calculate your chances, but it's meant to keep things fair across different test versions.
Results come immediately. The system generates a pass/fail notification right there on screen, which is both terrifying and relieving at the same time. Your official score report shows up in your AHIP account within a few business days, breaking down your performance by domain so you can see where you crushed it and where you struggled.
How the scoring actually works behind the scenes
The AHM-540 uses something called criterion-referenced scoring. Basically, they set a competency threshold based on subject matter expert input about what a qualified medical management professional should know. They don't curve the exam or limit the number of people who can pass. If everyone demonstrates competency, everyone passes.
Each question contributes to your overall score, but not equally. The psychometric folks at AHIP use item response theory to weight questions based on difficulty and discrimination power. Harder questions that separate competent candidates from struggling ones might carry slightly more weight, though they're never gonna tell you which ones those are during the exam.
No penalty for wrong answers. This is huge. If you're running out of time or really have no clue on a question, guess. An unanswered question is automatically wrong, but a guess gives you at least a chance. I've seen people leave questions blank out of some weird test-taking principle they learned in school, and it makes zero sense here.
My cousin took this exam twice, actually. First time he left eight questions blank because he "didn't want to guess wrong." Failed by what probably amounted to those eight questions. Second attempt he guessed on everything he didn't know and passed comfortably. Sometimes the old-school test advice just doesn't apply anymore.
Breaking down the domain weights
The AHM-540 exam objectives split across several major domains, and understanding these weights helps you focus your study time. Medical management foundations and utilization management typically make up the biggest chunks, probably 30-35% combined. If you're weak in UM processes, you're gonna have a bad time because that's where they really test whether you understand prior authorization workflows, concurrent review, and retrospective analysis.
Case management and care coordination usually account for another 20-25% of questions. This section trips up people who haven't actually worked in CM roles because the questions get into the nitty-gritty of care plan development, interdisciplinary team dynamics, and transitional care planning. Reading about it? Different from doing it.
Population health management and chronic condition programs show up heavily too. Expect questions about risk stratification methods, health promotion programs, and disease management program design. The exam loves asking about measuring outcomes and demonstrating ROI, which connects to quality improvement concepts.
Regulatory and compliance stuff rounds out maybe 10-15% of the exam. HIPAA, accreditation standards, medical necessity criteria, all fair game. These questions are often straightforward if you know the material, but they're also easy to overthink if you start doubting yourself.
Why people fail and how to avoid it
The AHM-540 exam difficulty sits somewhere in the moderate-to-challenging range, honestly. If you're working in utilization management or case management already, you've got a solid foundation. But if you're trying to break into medical management from another area, the terminology and conceptual frameworks can feel overwhelming.
Common failure points? Not understanding the distinction between utilization management vs case management. The exam will test whether you know when each approach applies. People also struggle with population health strategies because that requires systems-level thinking, not just individual patient care knowledge. And honestly, some folks underestimate how much you need to know about quality metrics and outcome measurement approaches.
Time management kills candidates too. You get a set number of questions (usually around 75-85) and a time limit that works out to roughly 90 seconds per question. Sounds like plenty until you hit a complex scenario question that requires reading three paragraphs of case information before you even see what they're asking. Practice your pacing.
What your score report tells you (and what it doesn't)
After you pass, your score report shows domain-level performance. You'll see something like "Utilization Management: Proficient" or "Case Management: Needs Improvement." These descriptors give you a sense of relative strength, but they won't tell you your exact percentage in each area or which specific questions you missed.
If you fail, the report becomes more valuable for targeting your restudy efforts. Pay attention to which domains you scored lowest in and focus your prep there. Don't just reread everything, that's inefficient. Drill into your weak areas with focused practice and deeper study of those specific concepts.
The AHM-540 (Medical Management) credential itself doesn't expire in the traditional sense, but AHIP recommends staying current with continuing education. Some employers require periodic renewal or completion of updated coursework, especially as medical management practices evolve with value-based care models and new technologies.
Retake policies and costs
If you don't pass, you can retake the exam after a waiting period, usually 30 days minimum. The AHM-540 exam cost for a retake is the same as the initial attempt, which runs somewhere around $250-300 depending on whether you're buying just the exam or bundling it with study materials. Check the current AHIP pricing because it changes.
Some organizations offer exam vouchers or bulk pricing if multiple employees are pursuing AHIP certifications. Worth asking your employer about reimbursement policies before you pay out of pocket. Many health plans and managed care organizations see enough value in the AHM-250 (Healthcare Management: An Introduction) and AHM-540 credentials that they'll cover costs.
You typically get three attempts within a 12-month period before you have to wait a full year to try again. This rarely comes up because most people either pass on attempt one or two, or they realize they need way more preparation and take time to build their knowledge base properly.
Score interpretation for career planning
Passing is passing. There's no distinction between someone who barely cleared the threshold and someone who crushed it with a near-perfect score. Your credential looks the same either way. That said, how you perform can tell you where you're really strong versus where you memorized enough to squeak by.
If you passed but struggled with quality improvement concepts, that's a signal to pursue additional training in that area before taking on roles with heavy QI responsibilities. The AHM-540 works well as part of a broader certification path. Candidates often pair it with AHM-520 (Health Plan Finance and Risk Management) or AHM-530 (Network Management) depending on their career trajectory.
Use your score report strategically. Not gonna lie, the domains where you scored highest are probably where you should focus your job search or internal transfer requests initially. Build credibility in your strong areas while developing competency in weaker ones through on-the-job learning and targeted professional development.
Conclusion
Wrapping up: is the AHIP AHM-540 Medical Management exam right for you?
Real talk here.
If you're working in utilization management, care coordination, or population health, or you want to break into those roles, the AHIP AHM-540 Medical Management certification is absolutely worth the time and money. it's another checkbox on your resume. This credential actually validates that you understand the medical management concepts in health plans that employers are looking for, from utilization review workflows to quality improvement metrics. It also signals you've got the clinical judgment and operational know-how that separates serious professionals from folks just collecting letters after their name.
The exam is not easy though.
Not gonna lie, the AHM-540 exam difficulty tends to catch people off guard if they underestimate the breadth of content. You're dealing with everything from regulatory compliance to chronic condition management strategies, and the questions test application, not just recall. That's why AHM-540 study materials matter so much. Cramming the night before won't cut it, period. You need structured prep, ideally 3-4 weeks if you've got relevant experience. Longer if this is new territory for you.
The AHM-540 passing score is set by AHIP based on exam performance data, and while they don't publish the exact number, you'll need to demonstrate solid competency across all exam objectives. Given the AHM-540 exam cost (which varies but typically runs a few hundred dollars), you really don't want to wing it and pay retake fees. I've seen too many people skip practice tests and then regret it when they see how specific the scenarios can get. Mixed feelings here because some folks do pass without extensive prep, but why gamble?
Speaking of practice tests, this is where most successful candidates get their edge. You can read the official materials all day, but until you're answering questions under timed conditions, you won't know where your weak spots are. The difference between utilization management vs case management might seem clear in theory, but exam questions love to blur those lines in realistic health plan scenarios that'll make you second-guess yourself. Kind of like how I thought I had diabetes management protocols nailed until a practice question threw in a dual-diagnosis patient with behavioral health comorbidities and suddenly I was rereading my notes at 11 PM on a Tuesday.
If you're serious about passing on your first attempt, I would strongly recommend checking out the AHM-540 Practice Exam Questions Pack. It's designed to mirror the actual exam format and covers the full range of topics you'll face: population health management strategies, care coordination protocols, quality metrics, all of it. Practice questions are probably the best investment you can make alongside your study time, especially if you're balancing exam prep with a full-time job.
Bottom line?
The AHM-540 prerequisites are minimal, but the knowledge requirements are not. Go in prepared, use quality resources, and you'll walk out with a credential that actually opens doors in medical management careers.
Show less info
Comments
Hot Exams
Related Exams
Associate - Cloud Infrastructure and Services v4 Exam
Specialist - Technology Architect Midrange Storage Solutions Exam
CompTIA Network+ Exam
Implementing Cisco Application Centric Infrastructure - Advanced (DCACIA)
SAFe Release Train Engineer (RTE)
Certified Fraud Examiner
Enterprise Geodata Management Professional 2201
Tableau Desktop Specialist
SuiteFoundation Certification Exam SuiteFoundation Certification
SAP Certified Technology AssociateSAP Process Orchestration
Implementing Cisco Collaboration Cloud and Edge Solutions (300-820 CLCEI)
Healthcare Management: An Introduction
Medical Management
Health Plan Finance and Risk Management
Network Management
Governance and Regulation
How to Open Test Engine .dumpsarena Files
Use FREE DumpsArena Test Engine player to open .dumpsarena files

DumpsArena.co has a remarkable success record. We're confident of our products and provide a no hassle refund policy.

Your purchase with DumpsArena.co is safe and fast.
The DumpsArena.co website is protected by 256-bit SSL from Cloudflare, the leader in online security.