AHM-510 Practice Exam - Governance and Regulation
Reliable Study Materials & Testing Engine for AHM-510 Exam Success!
Exam Code: AHM-510
Exam Name: Governance and Regulation
Certification Provider: AHIP
Certification Exam Name: AHIP Certification

Free Updates PDF & Test Engine
Verified By IT Certified Experts
Guaranteed To Have Actual Exam Questions
Up-To-Date Exam Study Material
99.5% High Success Pass Rate
100% Accurate Answers
100% Money Back Guarantee
Instant Downloads
Free Fast Exam Updates
Exam Questions And Answers PDF
Best Value Available in Market
Try Demo Before You Buy
Secure Shopping Experience
AHM-510: Governance and Regulation Study Material and Test Engine
Last Update Check: Mar 19, 2026
Latest 76 Questions & Answers
45-75% OFF
Hurry up! offer ends in 00 Days 00h 00m 00s
*Download the Test Player for FREE
Dumpsarena AHIP Governance and Regulation (AHM-510) Free Practice Exam Simulator Test Engine Exam preparation with its cutting-edge combination of authentic test simulation, dynamic adaptability, and intuitive design. Recognized as the industry-leading practice platform, it empowers candidates to master their certification journey through these standout features.
What is in the Premium File?
Satisfaction Policy – Dumpsarena.co
At DumpsArena.co, your success is our top priority. Our dedicated technical team works tirelessly day and night to deliver high-quality, up-to-date Practice Exam and study resources. We carefully craft our content to ensure it’s accurate, relevant, and aligned with the latest exam guidelines. Your satisfaction matters to us, and we are always working to provide you with the best possible learning experience. If you’re ever unsatisfied with our material, don’t hesitate to reach out—we’re here to support you. With DumpsArena.co, you can study with confidence, backed by a team you can trust.
AHIP AHM-510 Exam FAQs
Introduction of AHIP AHM-510 Exam!
AHIP AHM-510 is a certification exam for health insurance professionals. It is designed to test the knowledge and skills of individuals who work in the health insurance industry. The exam covers topics such as health insurance regulations, health care reform, health insurance products, and health care delivery systems.
What is the Duration of AHIP AHM-510 Exam?
The AHIP AHM-510 exam is a 90-minute exam consisting of 75 multiple-choice questions.
What are the Number of Questions Asked in AHIP AHM-510 Exam?
There are a total of 75 questions on the AHIP AHM-510 exam.
What is the Passing Score for AHIP AHM-510 Exam?
The passing score required for the AHIP AHM-510 exam is 80%.
What is the Competency Level required for AHIP AHM-510 Exam?
The AHIP AHM-510 exam is designed to assess the knowledge and skills of individuals who are seeking to become certified as a Health Insurance Professional. The exam covers topics such as health insurance plans, benefits, and regulations. To pass the exam, individuals must demonstrate a basic understanding of the health insurance industry and demonstrate the ability to apply the knowledge to real-world scenarios. The minimum competency level required to pass the AHIP AHM-510 exam is a high school diploma or equivalent.
What is the Question Format of AHIP AHM-510 Exam?
The AHIP AHM-510 exam consists of multiple-choice, drag and drop, and build list questions.
How Can You Take AHIP AHM-510 Exam?
The AHIP AHM-510 exam can be taken either online or at a testing center. To take the exam online, you will need to register on the AHIP website and purchase the exam. Once you have registered, you will be able to access the exam, which is timed and must be completed within the allotted time. To take the exam at a testing center, you will need to contact your local AHIP testing center to schedule an appointment. You will then need to bring a valid identification with you to the testing center on the day of your exam.
What Language AHIP AHM-510 Exam is Offered?
The AHIP AHM-510 exam is offered in English only.
What is the Cost of AHIP AHM-510 Exam?
The AHIP AHM-510 exam is offered for a fee of $125.
What is the Target Audience of AHIP AHM-510 Exam?
The target audience of the AHIP AHM-510 Exam are healthcare professionals who have completed a health insurance certification program and wish to become certified as a Health Insurance Professional. This certification is designed for individuals who work in the healthcare industry and wish to expand their knowledge and skills.
What is the Average Salary of AHIP AHM-510 Certified in the Market?
The average salary for professionals with an AHIP AHM-510 certification varies depending on the job market, the organisation and the individual's experience. Generally, salaries for those with this certification range from $60,000 to $80,000 per year.
Who are the Testing Providers of AHIP AHM-510 Exam?
AHIP does not offer testing for AHM-510 exam directly. However, AHIP does partner with Prometric, a leading testing and certification provider, to offer the AHM-510 exam.
What is the Recommended Experience for AHIP AHM-510 Exam?
The recommended experience for taking the AHIP AHM-510 exam is having a minimum of three years of healthcare experience, including two years in a leadership role. Candidates should also have an understanding of healthcare finance, economics, and policy. Additionally, it is suggested that the candidate have a general knowledge of the U.S. healthcare system.
What are the Prerequisites of AHIP AHM-510 Exam?
The AHIP AHM-510 exam requires that the candidate have a minimum of one year of experience in the health insurance industry, or have completed an AHIP-approved health insurance training program.
What is the Expected Retirement Date of AHIP AHM-510 Exam?
The official website to check the expected retirement date of AHIP AHM-510 exam is https://www.ahip.org/ahip-exams/ahm-510/.
What is the Difficulty Level of AHIP AHM-510 Exam?
The AHIP AHM-510 exam is considered to be of moderate difficulty level. The exam consists of multiple-choice questions and is designed to test the knowledge and skills of a candidate in the field of health insurance and managed care.
What is the Roadmap / Track of AHIP AHM-510 Exam?
AHIP AHM-510 Exam is a certification track/roadmap for healthcare professionals. It is designed to help them gain the knowledge and skills necessary to effectively manage healthcare organizations. The exam covers topics such as healthcare finance, operations, quality, and compliance. It also covers topics related to healthcare information technology, including data security, privacy, and electronic health records.
What are the Topics AHIP AHM-510 Exam Covers?
The AHIP AHM-510 exam covers the following topics:
1. Health Care Delivery System: This section of the exam covers the various components of the health care delivery system, including the roles of providers, payers, and other stakeholders. It also covers the regulatory and legal environment of health care, as well as the impact of technology on the system.
2. Health Care Finance: This section of the exam covers the fundamentals of health care finance, including reimbursement and payment models, as well as the financial management of health care organizations.
3. Health Care Quality and Performance Improvement: This section of the exam covers the various aspects of quality and performance improvement in health care, including the use of data and analytics, as well as strategies for improving quality and performance.
4. Health Care Risk Management: This section of the exam covers the fundamentals of risk management in health care, including the identification, assessment, and mitigation of risks.
5.
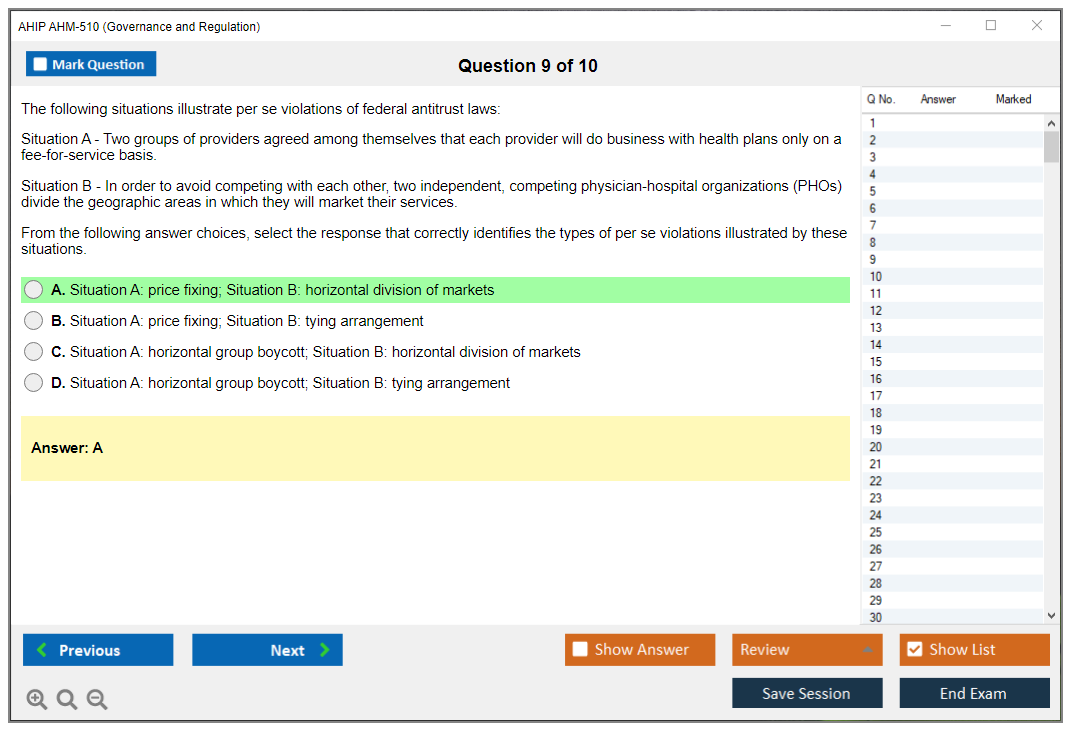
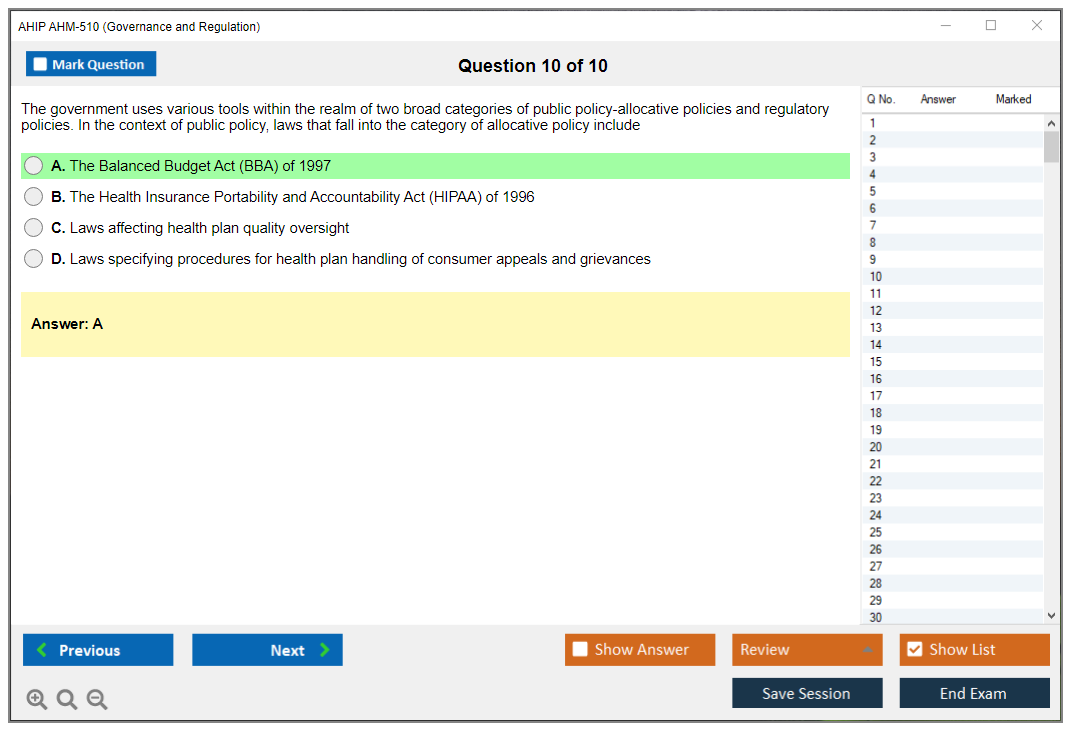
What are the Sample Questions of AHIP AHM-510 Exam?
1. What are the four main components of a health plan's risk adjustment program?
2. How do medical coding systems help health plans identify patient care services?
3. What is the difference between a preferred provider organization (PPO) and a health maintenance organization (HMO)?
4. What is the purpose of a health care utilization review?
5. What are the common types of fraud and abuse in the health care industry?
6. What are the key components of a health plan's quality improvement program?
7. What is the difference between a fee-for-service plan and a managed care plan?
8. What are the basic principles of health care cost containment?
9. What is the purpose of a health care provider network?
10. How do health plans use data analytics to improve patient outcomes?
AHIP AHM-510 (Governance and Regulation) Overview Understanding what this certification actually does for your career Look, the AHM-510 Governance and Regulation credential isn't some general compliance cert you can slap on your resume next to a dozen others. It's built specifically for health insurance professionals who work in compliance, regulatory affairs, and governance roles at managed care organizations and health plans. Basically the folks who actually live in the regulatory trenches day after day dealing with requirements that seem to multiply overnight. I mean, if you're a compliance officer trying to work through the absolute maze of federal and state regulations, this validates that you actually know what you're doing beyond just reading policy memos. What makes this different? It demonstrates competency in implementing effective governance structures and compliance programs that are unique to the payer side of healthcare. Provider compliance is one thing. Health plan... Read More
AHIP AHM-510 (Governance and Regulation) Overview
Understanding what this certification actually does for your career
Look, the AHM-510 Governance and Regulation credential isn't some general compliance cert you can slap on your resume next to a dozen others. It's built specifically for health insurance professionals who work in compliance, regulatory affairs, and governance roles at managed care organizations and health plans. Basically the folks who actually live in the regulatory trenches day after day dealing with requirements that seem to multiply overnight. I mean, if you're a compliance officer trying to work through the absolute maze of federal and state regulations, this validates that you actually know what you're doing beyond just reading policy memos.
What makes this different? It demonstrates competency in implementing effective governance structures and compliance programs that are unique to the payer side of healthcare. Provider compliance is one thing. Health plan regulatory requirements are a completely different animal with layers of state insurance department oversight, ERISA fiduciary duties, and CMS requirements all stacked on top of each other.
Honestly, this credential matters most for compliance officers, regulatory analysts, and health plan administrators who need to prove they understand both the corporate governance principles and the regulatory frameworks that govern managed care organizations. It's part of AHIP's full certification portfolio for health insurance professionals. It carries weight when you're dealing with state insurance departments or federal regulators because they know exactly what knowledge base it represents. They've probably seen it on enough resumes to recognize it means something real.
The regulatory space you'll need to master
Federal regulatory requirements form the backbone of what AHM-510 (Governance and Regulation) covers. You're looking at ERISA, HIPAA, the ACA, Medicare regulations, Medicaid managed care rules. Basically every major federal framework that touches health insurance operations, which is a lot more than most people realize when they first dive into health plan compliance. But here's where it gets tricky: state insurance department oversight adds another entire layer of complexity with licensure requirements, market conduct regulations, and state-specific mandates that vary wildly depending on where your health plan operates.
Corporate governance principles? They go deep.
Not gonna lie, understanding the difference between fiduciary oversight in a publicly traded health plan versus a nonprofit Blues plan versus a Medicaid MCO requires nuanced knowledge that you won't pick up from generic corporate governance courses. Board of directors responsibilities and fiduciary duties aren't just theoretical concepts here. They're practical frameworks you'll actually use when preparing board materials or responding to regulatory inquiries about governance structures.
Compliance program structure gets granular. Monitoring protocols, auditing methodologies, corrective action processes, and how to actually document everything so it holds up during a regulatory examination. The thing is, risk management frameworks and enterprise risk assessment methodologies are covered extensively because regulators expect health plans to have sophisticated approaches to identifying and mitigating compliance risks before they become consent orders or civil monetary penalties that make the news.
You'll also tackle regulatory reporting requirements with all their filing deadlines and documentation standards. Ethics policies. Conflict of interest management, and corporate integrity agreements that come into play when a health plan has previous enforcement history. The AHM-250 (Healthcare Management: An Introduction) provides foundational context, but AHM-510 goes way deeper into the regulatory weeds. Like, really deep.
I once sat through a three-hour board meeting where we spent forty-five minutes just debating the language in a single attestation form for state filing. That's the level of detail this world operates on.
Who actually needs this certification
Compliance officers? Obviously. Regulatory affairs professionals in health insurance companies are the natural candidates. But legal counsel specializing in healthcare regulation and managed care law increasingly pursue this because it demonstrates practical knowledge of how regulations actually get implemented, not just theoretical legal interpretation you'd get from law school.
Health plan executives responsible for governance and regulatory oversight benefit from this credential when they're interfacing with boards of directors or testifying before state insurance commissioners. Situations where credibility matters more than you might think. Quality assurance managers implementing compliance monitoring programs use the frameworks taught in AHM-510 to structure their audit protocols and risk assessments.
Government affairs specialists working with state and federal regulators find value here, though it's not always obvious at first glance. Consultants advising health plans on regulatory compliance strategies use it to demonstrate specialized expertise that separates them from general healthcare consultants. Internal auditors evaluating governance effectiveness need to understand what "good" looks like from a regulatory perspective. This certification establishes that benchmark in ways that internal experience alone can't always communicate. Risk management professionals in managed care organizations round out the typical candidate pool, though I've seen claims professionals and even network managers pursue it when moving into compliance-adjacent roles. The career paths in health insurance can be surprisingly fluid if you're strategic about it.
How this credential moves your career forward
Enhanced credibility? Absolutely real. When you're responding to a market conduct examination or explaining your compliance program structure to a CMS auditor, having AHM-510 signals that you speak their language and understand the regulatory expectations without needing everything translated into layperson terms first.
Competitive advantage for compliance and regulatory affairs positions is real. HR departments and hiring managers in health insurance use AHIP certifications as screening criteria because they know the knowledge requirements and can filter candidates more efficiently. The foundation for advancement to chief compliance officer or regulatory director roles often includes demonstrated expertise in complex health insurance regulatory environments. This certification provides that documentation in a way that job experience alone sometimes doesn't convey to people outside your organization who are evaluating your qualifications.
I mean, recognition by employers as evidence of specialized governance knowledge matters more than you might think initially. Generic compliance certifications like CHC or CCEP? They're valuable, don't get me wrong, but they're healthcare-wide. AHM-510's health insurance-specific focus gives you something different. The emphasis on managed care governance structures, the coverage of both commercial and government program regulatory requirements. It all makes this directly applicable to health plan operations in ways that broader certifications aren't. It's the difference between understanding hospitals versus understanding payers, which are fundamentally different beasts.
Networking opportunities with other certified health insurance professionals and increased earning potential in compliance and regulatory career tracks are secondary benefits, but they're worth mentioning because they're not insignificant. Look, compliance roles at health plans can pay well, especially at the director and VP levels, and credentials that validate specialized expertise help justify those compensation levels when you're negotiating offers or asking for promotions.
The certification integrates nicely with AHM-520 (Health Plan Finance) and AHM-530 (Network Management) if you're building full health plan operational expertise. Honestly, that combination makes you pretty well-rounded from an operational perspective. Or combines with AHM-540 (Medical Management) if you're focused on clinical compliance and quality oversight instead.
AHM-510 Exam Objectives and Content Domains
The AHIP AHM-510 exam is basically a "can you keep a health plan out of trouble" test, with a heavy dose of governance, regulation, and day-to-day oversight. Real talk.
If you've worked in operations, compliance, internal audit, risk, legal, or even provider contracting, a lot of this'll feel familiar. If you haven't, honestly, it can feel like learning two languages at once: board-level controls plus government program rules plus state DOI expectations all smooshed together.
What the exam is really testing
Think of the AHM-510 exam objectives as a map of who has authority, what rules apply, and how a plan proves it did the right thing when regulators come knocking with their clipboards and attitude. Some topics are "define the rule." Many are "apply it in a messy scenario," like a delegated vendor messing up claims, or a board packet missing the documentation that would've saved everyone during an exam. That particular nightmare keeps compliance officers up at night.
The domains aren't equal. Domain weights matter. I mean, you can't spend all week memorizing small reporting details and ignore governance and federal regulation, because those sections are where the exam actually lives.
Domain 1: Corporate governance structures and board oversight (25-30%)
This domain is board mechanics and accountability. Not vibes. You need to know composition requirements for health insurance company boards, what independence means in practice, and how conflict of interest policies are supposed to work when a director also has business ties.
Fiduciary duties are a big deal here: care, loyalty, and obedience. Duty of care is the "show your work" one. Read the materials, ask questions, document decisions, and don't rubber-stamp management just because everyone's tired and wants to go home. Duty of loyalty is conflicts, self-dealing, related-party transactions. Duty of obedience is staying aligned with law, charter, and mission, which shows up when a plan starts stretching into risky products without the right approvals.
Committee structures come up constantly. Audit, compliance, risk, compensation. Expect questions about charters, meeting cadence, and what gets escalated to the full board versus what dies in subcommittee. Board meeting requirements matter too. Quorum rules. Minutes. Retention. Documentation standards. Fragments. Paper trails. The stuff nobody wants to do but everybody needs later.
Executive compensation governance can show up with regulatory limitations and how boards approve incentives without accidentally paying for bad behavior. Subsidiary governance matters for affiliated entities, especially when you've got an insurance company plus an admin services org plus delegated provider groups all under one messy umbrella. Someone has to oversee the whole thing, and the exam wants you to recognize when governance gets too fragmented or when accountability just evaporates into the org chart.
NAIC Model Acts and "best practice" governance concepts appear as reference points, plus board education expectations and ongoing training. Governance metrics and board effectiveness evaluations. Boring? Yes. Testable? Also yes.
Domain 2: Federal regulatory framework for health insurance (30-35%)
This is the biggest slice, and it's the one that makes the exam feel wide. ACA market reforms and essential health benefits. HIPAA privacy and security. ERISA for employer-sponsored plans and fiduciary responsibilities. Medicare Advantage and Part D with CMS oversight. Medicaid managed care with state-federal dynamics that never quite sync up perfectly. Mental Health Parity. No Surprises Act. Consolidated Appropriations Act transparency rules. Anti-fraud statutes like the False Claims Act and Anti-Kickback Statute. And then enforcement: penalties, corrective action plans, and what happens when regulators say "prove you fixed it" and you have 30 days to produce documentation that may or may not exist.
If you want one area to over-prepare, it's Medicare Advantage and Part D oversight concepts and how federal enforcement works, because the questions tend to be scenario-based and they stack rules on top of each other like regulatory Jenga. Look, HIPAA questions often read easy, but the tricky part is operationalizing it. Business associates, minimum necessary, security controls, incident response, and how a plan documents compliance when something goes sideways at 3 a.m. on a Saturday.
No Surprises and transparency requirements are newer compared with the classic statutes, so people underestimate them. Don't. The exam likes real-world administration details, like independent dispute resolution concepts and what information gets disclosed and when and to whom.
Actually, side note: if you've ever sat through a transparency reporting project, you know the data doesn't live in one system. It's scattered across claims, contracts, provider files, and half-baked spreadsheets someone built in 2017. The regulations assume clean data pipelines. The reality is archaeological digs through legacy systems. But I digress.
Domain 3: State insurance regulation and market conduct (20-25%)
State regulation is where the department of insurance shows up with very specific ideas about how you should run your business. Licensure and certificates of authority. Rate filing and actuarial certification. Form filing for policies, contracts, and member materials. Market conduct exams. Network adequacy. Prompt pay. External review for denials. Producer licensing and appointments. Unfair trade practices and consumer protection.
Multi-state operations? Absolute headache. One plan, many states, many different definitions of "timely," "adequate," "material change," and "approval required." NAIC accreditation standards and model law adoption patterns show up as the backdrop for why states look similar but never identical, which is both fascinating and maddening depending on your role.
One sentence: market conduct is operational truth serum.
Domain 4: Compliance program development and implementation (15-20%)
This is classic compliance architecture. The seven elements, the compliance officer's role and reporting line, written policies and procedures, code of conduct, training design for different audiences, and communication channels like anonymous hotlines that people actually need to trust.
Monitoring and auditing methods are where people get lost, because the exam expects you to know the difference between ongoing monitoring, periodic audits, and investigations, and how you document each one so it holds up later when someone's digging through your files. Corrective action plans and remediation strategies matter. Plus compliance committee structure and meeting frequency. Vendor and business associate oversight is part of health insurance governance compliance, because the thing is the plan owns outcomes even when work is delegated to someone three contracts removed.
Integration with enterprise risk management. Not optional.
Domain 5: Risk assessment and internal controls (10-15%)
ERM frameworks, risk identification (environmental scanning), and prioritization using likelihood and impact matrices. Control design. Implementation. Operational controls for claims, enrollment, member services. Financial controls for premium collection and medical loss ratio. InfoSec controls for breach prevention. Third-party risk management for delegated arrangements. Key risk indicators. Risk monitoring. Reporting to the board and senior management.
This is the "prove you control the machine" domain. Short sentences work. Lots of them.
Domain 6: Regulatory reporting and government relations (5-10%)
Smaller weight, but easy points if you're organized and methodical. Annual and quarterly filings. Statutory accounting basics. Quality reporting like HEDIS and Stars. Fraud waste and abuse reporting. Incident reporting. Material transaction notifications. Program reporting for Medicare and Medicaid contracts. Add transparency reporting, exam responses, and regulator communication practices that don't make things worse.
Also, document production. Timelines. Version control. Painful stuff nobody celebrates but everybody needs.
Quick answers people ask while building an AHIP AHM-510 study guide
How much does the AHM-510 exam cost? It changes, so check AHIP's current listing, because employer discounts and bundles can shift pricing in ways that matter to your budget. What is the AHM-510 passing score? AHIP sets scoring policy, and they can adjust it, so verify in the candidate handbook rather than trusting random forum posts from 2019. How hard is it? If you've done managed care regulation training or worked with health plan regulatory requirements, it's fair but broad, and breadth is what gets you when you're tired at question 87.
Best materials? Start with official course content, then add an AHM-510 practice test only if it explains answers, not just letter choices, because memorizing "C" doesn't teach you anything. As for AHM-510 prerequisites and AHM-510 renewal requirements, treat them like policy questions: confirm on AHIP's site, because eligibility and maintenance rules can change year to year for any AHIP certification for health insurance program, and you don't want to study the wrong thing for the right credential or vice versa.
AHM-510 Exam Cost, Registration, and Logistics
What you're actually paying for the AHM-510
Here's the deal. The standard exam fee sits between $325 and $425 depending on whether you've got AHIP membership. Non-members pay the higher end of that range, which adds up fast if you're planning to knock out multiple certifications in the governance and compliance space. AHIP members get discounted pricing that can shave off $50 to $100 per exam, but that membership itself costs money annually, so you need to do the math on whether you're coming out ahead or just shuffling dollars around.
Course materials? Sold separately. The official AHIP course bundle typically includes your exam voucher plus study materials, running somewhere between $500 and $700 total. That's a chunk of change, but the bundle route gives you everything in one package without hunting down materials piecemeal. Who has time for that? If you're registering through an organization, group discounts kick in when multiple people from the same employer sign up, which can bring per-person costs down noticeably.
Retake fees are real. If you don't pass on your first attempt, you're looking at another fee that's usually comparable to the initial exam cost. Some testing providers charge separately for remote proctoring services, though most roll that into the base fee now. Hidden fees aren't much of a problem, but always confirm what's included before you register.
Membership math that actually matters
Annual AHIP membership runs a few hundred dollars depending on your professional category. The benefits include exam discounts, member-only resources, webinars, and access to networking events that can be really useful if you're building a career in managed care regulation. If you're planning to pursue multiple AHIP certifications like AHM-520 (Health Plan Finance and Risk Management) or AHM-540 (Medical Management) within the same year, the membership discount can offset your annual dues pretty quickly. Sometimes it's the only financially smart move.
Here's my decision framework: taking one exam this year? Probably skip membership. Planning three or more certifications? Membership pays for itself. You also get access to compliance updates and regulatory change alerts that are current, which matters when you're working in governance roles where staying informed isn't optional. It's your job.
My first certification year, I skipped the membership thinking I'd save money. Took two exams, paid full price for both, then did the math later and realized I'd basically donated an extra hundred bucks to AHIP for no reason. Live and learn.
Getting yourself registered
Creating an account on the AHIP certification portal takes maybe five minutes. You'll select AHM-510 (Governance and Regulation) from their certification catalog and choose between the course bundle or exam-only registration. Payment methods include credit cards and organizational purchase orders, which helps if your employer's footing the bill but requires their procurement process. Bureaucracy, right?
Confirmation emails usually arrive within a few hours, and if you bought the course bundle, you get immediate access to study materials through the portal. Your exam voucher activates right away but has an expiration period, typically six months to a year from purchase, so don't register way too early if you're not ready to commit to a study timeline. The scheduling window opens as soon as your voucher is active, giving you flexibility to book when you're prepared instead of panicking at the last minute.
Booking your actual test date
AHIP uses PSI or Pearson VUE for testing delivery, depending on their current provider contract. You can test at physical testing centers or take the exam remotely through online proctoring. The testing center locator tool shows availability calendars, but scheduling at least two to three weeks out is smart if you want your preferred date and time. Popular slots disappear faster than you'd think. Some locations offer evening and weekend slots, which is clutch if you're working full-time and can't take a weekday off.
Remote proctored exams give you convenience but require a quiet space, stable internet, and a webcam setup that meets their technical requirements. You'll get a confirmation email with what to bring (or not bring) on exam day, plus instructions for checking in.
When plans change
Look, life happens. Rescheduling without penalty requires 48 to 72 hours advance notice typically. Miss that window and you're paying a rescheduling fee that can run $50 to $100. Cancellation and refund policies exist for genuine emergencies, but they're strict. Documentation is usually required, and you're not getting a full refund even with approved circumstances.
Voucher extensions are sometimes available if you can't test within your validity period due to documented reasons. No-show situations result in forfeiture of your exam fee entirely, which is brutal but understandable from their perspective. Weather-related closures or emergency situations at testing centers trigger automatic rescheduling without penalties.
If you need to take it again
Most AHIP exams allow multiple attempts within a rolling timeframe, but waiting periods between attempts typically range from 30 to 90 days. Retake fees generally match or come close to the initial exam cost, so failing gets expensive fast. We're talking potentially over a thousand dollars if you're not careful. You'll receive a score report showing performance by domain, which gives you concrete data on where to focus your study efforts before the next attempt rather than just guessing what went wrong.
Maximum lifetime attempts exist for some credentials, though AHM-510 typically allows enough tries that it's not a practical concern unless something's wrong with your preparation approach.
Accommodations for testing accessibility
ADA accommodation requests require documentation from a qualified professional and should be submitted well in advance. Think 4 to 6 weeks minimum for approval processing. Extended testing time is the most common accommodation, along with separate testing rooms for candidates who need reduced distractions. Screen reader compatibility exists for visual impairments, and testing centers maintain accessibility features for physical disabilities. The accommodation approval timeline matters because you can't schedule your exam until accommodations are confirmed and in the system, so plan accordingly or you'll be waiting around frustrated.
AHM-510 Exam Format, Passing Score, and Results
Quick overview of what this exam is
The AHIP AHM-510 exam is the Governance and Regulation checkpoint a lot of health plan folks take when they want proof they understand oversight, compliance, and how regulators actually think. Not a vibes test, honestly. It's policies, accountability, and what happens when you screw up.
Governance is people and power. Regulation? Rules and receipts. Compliance is the paper trail.
What AHM-510 covers day to day
For AHM-510 Governance and Regulation, expect the exam to circle around board roles, delegated oversight, required reporting, and how internal controls are supposed to work when the plan's under pressure. You'll also see the "why" behind health plan regulatory requirements, like what state departments of insurance care about versus what federal programs enforce, plus the basic logic of audits, corrective action plans, and risk scoring.
Who benefits most? Compliance analysts. Ops managers. Internal audit. Delegated entity oversight teams. And people moving into leadership who keep getting pulled into "can we do this?" meetings. If you're doing managed care regulation training at work, this exam lines up with that mental model.
Exam format and structure (what it looks like on test day)
The AHIP AHM-510 exam is multiple-choice, with four answer options per question. Total items usually land in the 75 to 100 range, depending on the form you get. Some questions are operational and count toward your score, and some are pretest items being field-tested for future exams, and honestly you won't know which is which, so treat every question like it matters.
It's computer-based testing with on-screen navigation. You can move forward and back, and you can mark questions for review and return before time expires, which is basically the only reason pacing is survivable for most people. No penalty for guessing. Answer everything. Every blank? Self-inflicted wound.
You'll get scratch paper or a digital notepad for quick math or tracking options. No reference materials. No notes. No "quick peek" at your AHIP AHM-510 study guide. Closed world.
Time limits and pacing (how not to panic)
Testing time? Two to three hours, typically. That means you should budget about 1.5 to 2 minutes per question if you want to finish without doing the last 15 questions like you're speed-running a bad video game.
Tutorial time usually doesn't count against the exam clock, so don't waste brainpower rushing that part, but also don't treat it like a break room. During the exam you'll have a clock display. Most systems give time warnings as you get close to the end.
My pacing rule is simple. First pass, keep moving. If a question's turning into a fight, mark it and move on, because spending six minutes to maybe get one point is a bad trade when the exam's designed to reward coverage and consistency. You need enough time later to do a thorough review of your marked items with a calmer brain. Second pass, work the marked ones. Third pass, only if time remains, re-check anything with "except," "most likely," or "best next step" wording.
Passing score requirements (what you're aiming for)
The AHM-510 passing score is reported on a scaled score system. Depending on the program and form, that can look like 0 to 100 or something like 200 to 800. The passing threshold's set by AHIP using psychometric analysis, not by how well the other people in your session did.
People throw around "70%" as a common target, and it's a decent mental anchor, but verify the current requirement in your candidate handbook because policies change and different forms can map raw-to-scaled differently. This is criterion-referenced scoring. Not a curve. Your score isn't affected by other test-takers. No partial credit on multiple-choice. One question, one scored outcome.
How scoring works (why scaled scores exist)
Under the hood, scoring's usually based on classical test theory or item response theory, then an equating process is applied so different exam versions are comparable. That matters because not every form has identical difficulty, so equating keeps the passing standard consistent across forms.
Only operational items count toward your final score. Pretest items are mixed in for future development. Your raw score's converted to a scaled score for reporting. Some score reports include domain-level performance feedback, but you won't get an item-by-item breakdown, and that's normal for certification exams because they protect the question bank.
Results timing and what you receive
For computer-based tests, you typically get an immediate preliminary pass/fail at the end. Official score reports usually show up within two to five business days in the AHIP candidate portal, and you'll often get an email when they're posted.
Score reports usually include your total scaled score, pass/fail status, and sometimes domain performance indicators. Keep a copy. Portals change. People lose access. It happens. Also, results are confidential, and score release follows AHIP's policies, so don't expect your employer to magically see it unless you share it or they use an approved verification channel.
How to read the score report without overthinking it
Scaled score tells you where you landed relative to the passing standard. Not "percentage correct" in a clean way. If you get domain categories like "below expectations," "meets expectations," or "exceeds expectations," use that as a retake map, not as an ego score.
If percentile rankings appear? They're just comparison data. Useful, but not the point. Passing scores typically remain valid for certification purposes under AHIP's rules, and if you're worried about AHM-510 renewal requirements, confirm current policy because some credentials have continuing education expectations and some don't, and the wording matters.
After you pass (career ops stuff)
You'll usually get a digital badge or certificate after processing, then you can download documents from your transcript area. Add it to LinkedIn and your resume, but use the designation correctly. AHIP has rules for certification marks. They do care.
Employers may use verification services, and your achievement often shows up on your AHIP transcript with other AHIP certification for health insurance items if you collect more later.
Cost, prep materials, and the questions people always ask
How much does the AHIP AHM-510 exam cost? The AHM-510 exam cost varies by training bundle, member status, and whether your employer's paying, so check the current AHIP listing when you register.
What're the best study materials for AHM-510 Governance and Regulation? Start with the official materials tied to the AHM-510 exam objectives, then add targeted practice. A decent AHM-510 practice test helps you spot weak domains fast. If you want extra reps, I've seen people pair their course work with the AHM-510 Practice Exam Questions Pack because it forces timing and recall under pressure. That's the whole game, really.
How hard is it? If you've done compliance, delegation oversight, audits, or health insurance governance compliance work, it's fair but detailed. If you're new, it feels like a wall of terminology and "who's accountable" scenarios. I remember my first compliance role where I thought "corrective action plan" meant fixing a typo in a memo. Turns out when a state regulator uses that phrase, they mean something closer to "restructure your entire oversight model or we'll restructure it for you." Big learning curve.
Does AHM-510 have prerequisites? Official AHM-510 prerequisites may be minimal, but recommended knowledge is real. You should understand how a health plan's structured and how healthcare compliance and oversight works operationally.
If you're retaking or just want to be efficient, do timed sets, review misses, then retake. Rinse, repeat. And if you want a plug-and-play option for extra drills, the AHM-510 Practice Exam Questions Pack is an easy add, especially when you're inside that final week and your brain's tired.
AHM-510 Difficulty Level and Study Time Requirements
What you're really getting into with this exam
Look, I'm not gonna sugarcoat this. The AHIP AHM-510 exam sits comfortably in the moderate to moderately-difficult range, but that assessment depends heavily on what you're bringing to the table. AHIP doesn't publicly disclose pass rates (because of course they don't), but from conversations with colleagues and proctors, first-time test-takers seem to land somewhere between 60-75% pass rates. Not terrible, honestly. But definitely not a walk in the park either.
The challenge here? it's memorizing regulations and calling it a day. This exam wants you to apply governance principles and regulatory knowledge to realistic scenarios. You'll see questions that essentially throw a compliance dilemma at you and ask you to prioritize actions or identify which regulation applies. That application layer trips people up.
Why AHM-510 earns its reputation
The sheer volume hits first. You're covering federal regulations, state-level requirements, and governance frameworks all at once. Medicare rules, Medicaid details, commercial plan compliance, reporting timelines, and specific numerical thresholds that you just have to commit to memory. Distinguishing between similar provisions is really tricky when you're dealing with overlapping federal and state authority, I mean.
And here's the kicker: healthcare regulations change constantly. Something you studied three months ago might've been updated by new guidance or legislation. Staying current isn't optional, it's baked right into the difficulty. The scenario-based questions demand multi-step reasoning too. You can't just recognize the right answer, you've gotta work through what happens first, second, and third in a compliance situation.
Professional experience makes a huge difference in perceived difficulty. If you've spent years in compliance or regulatory affairs, you'll find many concepts familiar, maybe even intuitive. But if you're transitioning from clinical work or operations without much regulatory exposure? Yeah, you're gonna need more runway. The thing is, even people who've been in healthcare for ages sometimes struggle with this exam if their day-to-day work hasn't touched the regulatory side. I watched a director with fifteen years in operations fail twice before finally passing on the third attempt. Experience helps, but it has to be the right kind of experience.
Carving out enough study time
Experienced compliance professionals with three or more years in the field typically need 40-60 hours spread over 4-6 weeks. That assumes you're already fluent in regulatory language and compliance frameworks.
For professionals with some regulatory exposure (say one to three years) budget 60-80 hours over 6-8 weeks. You know enough to have context, but you'll need time to fill gaps and deepen understanding.
Career changers or entry-level candidates should realistically plan for 80-120 hours over 8-12 weeks. I know that sounds like a lot. It is. But trying to compress that timeline significantly just increases your failure risk, and nobody wants to pay for a retake.
There's always a trade-off between intensity and duration. You could theoretically cram everything into three weeks of brutal study sessions, but your retention will suffer and you'll burn out. Extended timelines with consistent, moderate effort usually produce better results. More confidence walking into the exam room, honestly.
What affects your personal timeline
Your background matters enormously here. Did you study healthcare administration, public health, or law? That foundation helps. Are your current job responsibilities touching compliance or regulatory work daily? You're already practicing without realizing it. If you've knocked out other AHIP certifications like AHM-250 (Healthcare Management: An Introduction) or AHM-520 (Health Plan Finance and Risk Management), you've got foundational knowledge that transfers.
Learning preferences play a role too. Some people absorb material faster through reading, others need practice questions to cement concepts. Your access to quality study materials matters. Not all study guides are created equal, and if you're working with outdated materials or resources that don't align with current exam objectives, you're wasting precious hours.
Test-taking skills shouldn't be underestimated either. If you get anxious during exams or struggle with time management under pressure, factor that in.
Mistakes that sabotage your preparation
Relying purely on memorization without understanding why regulations exist is probably the most common mistake I see. The exam isn't asking you to recite definitions. It wants to know if you can apply them.
People also tend to focus almost exclusively on federal regulations and neglect state-level content, which absolutely shows up on the test. Inadequate practice with scenario-based questions is another killer. You can know the material backward and forward, but if you haven't practiced working through complex scenarios, you'll freeze when you see them.
Procrastinating and then cramming in the final week before your exam date? That's just asking for trouble. Spaced repetition over time beats marathon sessions every single time. Skipping practice tests entirely, or taking them but not reviewing why you got questions wrong..both are missed opportunities to identify weak areas while you still have time to fix them. And honestly, studying with outdated materials is worse than not studying at all because you're literally learning incorrect information.
Setting yourself up for success
Create a structured study schedule with specific objectives for each session. Don't just block out "study time." Know exactly what you're covering.
Use multiple methods. Reading helps. So do flashcards, practice questions, maybe even teaching concepts to someone else. Understanding beats memorization.
Take regular practice tests to surface knowledge gaps early. The AHM-510 Practice Exam Questions Pack at $36.99 gives you realistic scenario-based questions that mirror the actual exam format. Worth every penny for identifying weak spots before test day, I mean it.
Join study groups if you can find them, or at least grab an accountability partner who's also prepping. Update your materials to reflect recent regulatory changes. Check AHIP's official resources and supplement with current compliance publications.
Allocate extra time to domains where your practice performance is weak rather than just reviewing what you already know. Build in buffer time before your exam date for final review. Don't schedule the exam for the day after your last study session.
Walking into exam day with realistic expectations
You're gonna see some questions that feel unfamiliar even after thorough preparation. That's normal. The exam is designed to test edge cases and nuanced applications.
Manage your anxiety about ambiguous questions by trusting your preparation and using process of elimination when you're uncertain. Don't second-guess yourself excessively. Your first instinct is usually right. Keep a steady pace without dwelling too long on any single question.
Remember that passing doesn't require a perfect score, so don't let one tough question derail your confidence for the rest of the exam. Stay focused through mental fatigue, take the allowed breaks if you need them, and trust the hours you've put in.
If you're looking at other certifications in the AHIP series, consider how AHM-530 (Network Management) or AHM-540 (Medical Management) might complement your governance and regulation knowledge for a more complete credential set.
AHM-510 Prerequisites and Eligibility Requirements (~500 words)
The AHIP AHM-510 exam is the governance, regulation, and compliance checkpoint a lot of health plan people eventually run into. It's not a coding test. Not a memorization contest either. The thing is, it's closer to "do you understand how a health plan is supposed to be run, watched, documented, and corrected when things go sideways."
AHM-510 Governance and Regulation is basically about health insurance governance compliance in the real world: boards and committees, internal controls, audits, reporting lines, regulatory filings, and what happens when oversight is weak. One bad process. One sloppy vendor. One missed deadline. It adds up fast.
What you'll actually be tested on
Start with the AHM-510 exam objectives and treat them like your map, because the exam tends to reward people who can connect concepts across chapters rather than quote definitions. You'll feel that when questions start mixing operations, compliance, and oversight into one scenario that makes your brain work harder than expected.
Governance shows up as roles, accountability, escalation, and decision rights. Regulation is federal versus state, plus how a plan proves it's meeting health plan regulatory requirements. Compliance means program design, audits, monitoring, corrective actions, and documentation. Ethics and controls? They're the "how do you prevent dumb stuff" layer. Reporting mechanisms, conflicts, operational checks.
Cost and registration basics
People ask: How much does the AHIP AHM-510 exam cost? The honest answer is that AHM-510 exam cost changes depending on whether you're buying an AHIP course bundle, whether your employer has a pricing agreement, and whether you're purchasing a package that includes learning materials and an exam attempt. So don't trust random numbers on forums. Verify on the official AHIP site at checkout, because that's the only price that matters.
Registration's usually straightforward. Buy the course and exam. Get access to the materials. Then schedule within the allowed testing window. Read the fine print on refunds and rescheduling. One missed window and you're emailing support at 11:58 pm. I knew someone who lost access completely because they thought their testing window auto-extended. It didn't.
Passing score and format realities
Next big question: What is the passing score for AHM-510? The AHM-510 passing score is not something I'd guess at, and neither should you. AHIP sometimes explains scoring at a high level, but the current policy and what you see on your candidate screen is where to confirm it.
Format-wise, expect scenario-heavy multiple choice. Timing matters. Questions are often written to see if you understand governance logic, not whether you can spot a keyword. Score reports can be immediate or posted after completion depending on the platform and rules at the time.
Difficulty: why people struggle
How hard is the AHM-510 exam? It's "hard" if you've never sat in a compliance meeting or worked with audits, grievances, appeals, or delegated entities. It's "annoying" if you have experience but you skim the details, because the exam loves policy distinctions and governance roles that feel similar until you get tested on them and suddenly realize they're not interchangeable at all.
What makes it challenging? The mix of managed care regulation training topics with operations and oversight. You're not just learning laws. You're learning how healthcare compliance and oversight is documented, monitored, and enforced. Common mistakes include rushing scenario questions, ignoring the "best next step" wording, and studying only definitions while skipping process flow.
Prerequisites and who is eligible
Here's the good news: AHM-510 prerequisites are usually light in the "formal gatekeeping" sense. Most candidates don't need a degree in anything particular, and there's typically no requirement that you already hold another credential before you register. But the practical prerequisites? Real.
Recommended baseline knowledge includes how health plans are organized, what regulators care about, and why governance is more than a board meeting agenda. If you've touched compliance, operations, internal audit, delegated vendor oversight, credentialing, quality, or risk, you'll recognize the patterns fast. If you're brand new, plan extra study time and don't pretend you can wing it.
Suggested backgrounds that fit well: compliance analyst, health plan ops, provider network support, grievance and appeals, QA, internal controls, or anyone on a path toward AHIP certification for health insurance roles where regulation and oversight are daily work.
Study materials that won't waste your time
What are the best study materials for AHM-510 Governance and Regulation? Start with the official course content, period. Your AHIP AHM-510 study guide should be the backbone because it aligns to the test blueprint, and third-party notes can drift or oversimplify. Sometimes they just flat-out contradict what's current.
Beyond that, I like two add-ons. First, your own glossary of terms you keep messing up. Second, a one-page "governance flow" cheat sheet: who owns what, who reports to whom, which artifacts prove compliance, and what triggers audits or corrective action. Other helpful stuff: your plan's compliance policies if you can access them, basic federal and state regulator summaries, and internal audit templates.
Study time depends on experience. If you're in compliance already, 2 to 4 weeks is often enough. If you're coming from claims or customer service, give it 4 to 6 and do more scenario practice.
Practice tests: use them the right way
An AHM-510 practice test is useful only if you review why you missed questions. Don't just re-take until you memorize letter patterns. Do a loop: attempt, review rationales, map misses back to the AHM-510 exam objectives, then re-test weak areas under time pressure.
Where to find reliable practice exams? Stick to official sources first. If you use unofficial ones, be picky, because bad questions teach bad habits.
Renewal and maintaining the credential
Last common question: Does AHM-510 require renewal or continuing education? AHM-510 renewal requirements depend on how the credential is issued and what program rules apply at the time, and those policies can change. Check the current AHIP policy page and save a PDF copy for your records.
If renewal or CE applies, track dates in a calendar and keep completion certificates in one folder. One lapse. One forgotten email. Then you're re-buying access you didn't plan for.
Fast FAQs people keep asking
Cost varies by package and employer pricing. Confirm at purchase. Passing score? Verify with AHIP's current candidate info. Difficulty: moderate if you know governance and compliance, tougher if you don't. Best materials: official content first, then targeted notes and practice review. Retakes: policy varies, read it before you click "start exam."
Conclusion
Making sure you're actually ready
Look, here's the deal.
The AHIP AHM-510 exam isn't something you just show up for and wing. I mean, you could try, but that's honestly not gonna end well for anyone involved. The governance and regulatory side of health insurance is dense as hell: federal oversight layered with state-level regulations, compliance programs that need actual understanding (not just rote memorization), and real-world scenarios where knowing the difference between a board's fiduciary duty and operational management actually matters. A lot.
What trips people up? Treating this like a checklist exam. You can't just memorize definitions and expect to pass. The thing is, the questions pull from health plan regulatory requirements and managed care regulation training concepts, sure, but they're really testing whether you can apply them in messy situations. Can you spot a compliance gap when it's buried in a paragraph? Do you understand why certain reporting structures even exist? That's where the AHIP AHM-510 study guide materials help, but only if you're using them to build actual comprehension, not just.. I don't know, coverage for coverage's sake.
Don't skip the practice work
Honestly? Biggest mistake I see is people who read everything, feel confident, then absolutely bomb because they never tested themselves under real pressure.
The AHM-510 practice test experience shows you what you don't know. More importantly, how the exam actually phrases things (which can be wildly different from how you'd expect). Governance questions can be wordy. Super wordy. Regulatory scenarios require you to distinguish between similar-sounding requirements that look identical at first glance. You need reps.
I remember someone telling me they'd studied for three weeks straight, felt great going in, then hit question twelve and realized they'd prepared for the wrong kind of test entirely. Brutal way to learn that lesson.
If you've been following an AHIP certification for health insurance path, you know the AHM-510 passing score isn't published as a hard number by AHIP in all cases, which makes it even more critical to over-prepare rather than aim for "just enough." The AHM-510 exam cost is manageable compared to some certs, but failing and retaking? That costs you time and money and momentum. Not worth it when solid prep exists.
Get the right tools in your corner
The AHM-510 exam objectives are clear enough if you dig into them. Having question sets that mirror the actual format makes everything click faster, though. I'm not gonna lie, having access to scenario-based questions that cover healthcare compliance and oversight, health insurance governance compliance, and operational controls is what separates people who pass comfortably from people who stress through every single question like it's a personal attack.
Mixed feelings here, but if you want a structured way to drill weak areas and validate your readiness before test day, check out the AHM-510 Practice Exam Questions Pack. It's built for this exam, covers the full scope of governance and regulation content, and gives you the kind of practice that actually translates to exam performance.
You've put in the study time. Make sure it counts.
Show less info
Hot Exams
Related Exams
P1 Management Accounting
Qlik Sense Business Analyst Certification Exam - February 2021 Release
Designing and Implementing a Data Science Solution on Azure
SAP Certified Application AssociateSAP SuccessFactors People Analytics: Reporting 1H/2022
PRINCE2 Foundation (by Exin)
Certified Associate in Project Management (CAPM)®
Salesforce Certified Marketing Cloud Administrator
Databricks Certified Data Engineer Professional Exam
Implementing Cisco Service Provider VPN Services (300-515 SPVI)
Medical Management
Microsoft Azure Administrator
Governance and Regulation
Healthcare Management: An Introduction
Health Plan Finance and Risk Management
Medical Management
Network Management
How to Open Test Engine .dumpsarena Files
Use FREE DumpsArena Test Engine player to open .dumpsarena files

DumpsArena.co has a remarkable success record. We're confident of our products and provide a no hassle refund policy.

Your purchase with DumpsArena.co is safe and fast.
The DumpsArena.co website is protected by 256-bit SSL from Cloudflare, the leader in online security.